Breath Biopsy Conference 2020: Breath Biomarkers for Liver Disease
Published on: 24 Nov 2020
The third annual Breath Biopsy Conference took place on 10–11 November 2020, with one of the highlights of this year’s meeting being the session on Breath Biomarkers for Liver Disease.

The liver disease session included some of the most exciting recent research discussed at this year’s conference. The invited presentations from John Plevris (University of Edinburgh), Scott Friedman (Icahn School of Medicine at Mount Sinai) and Giuseppe Ferrandino (Owlstone Medical), covered potential new non-invasive methods for the diagnosing, monitoring and stratification of liver disease patients. Notably, the sessions repeatedly highlighted the relevance of limonene on breath as an exogenous volatile organic compound probe (EVOC® Probe) for liver disease.
All three speakers commented on the severity of the current need for accurate, non-invasive tests for the screening of liver disease. Over 100M people in the US and EU are affected by early stage liver diseases and detection methods are either invasive, produce unreliable results or rely on structural rather than functional changes to the liver. In many US states, more than 30% of the population is already thought to have non-alcoholic fatty liver disease (NAFLD). By 2030, more than 25M Americans could have non-alcoholic steatohepatitis (NASH) and this is expected to result in a 178% rise in hepatocellular carcinoma (HCC).
The first speaker, Dr Ferrandino presented the results of targeted and untargeted analysis of breath samples for liver disease detection. Published research had previously suggested that limonene could be a valuable breath biomarker for liver disease as it is elevated in cirrhosis and falls following liver transplant. In a recently published study, Dr Ferrandino and his colleagues analyzed healthy and cirrhotic samples using Breath Biopsy. The data were used to produce a predictive model that could differentiate patients with cirrhosis from controls with 77% accuracy. The results also correlated with disease severity and blood biomarkers of liver function indicating the potential for limonene as an EVOC Probe for liver disease.
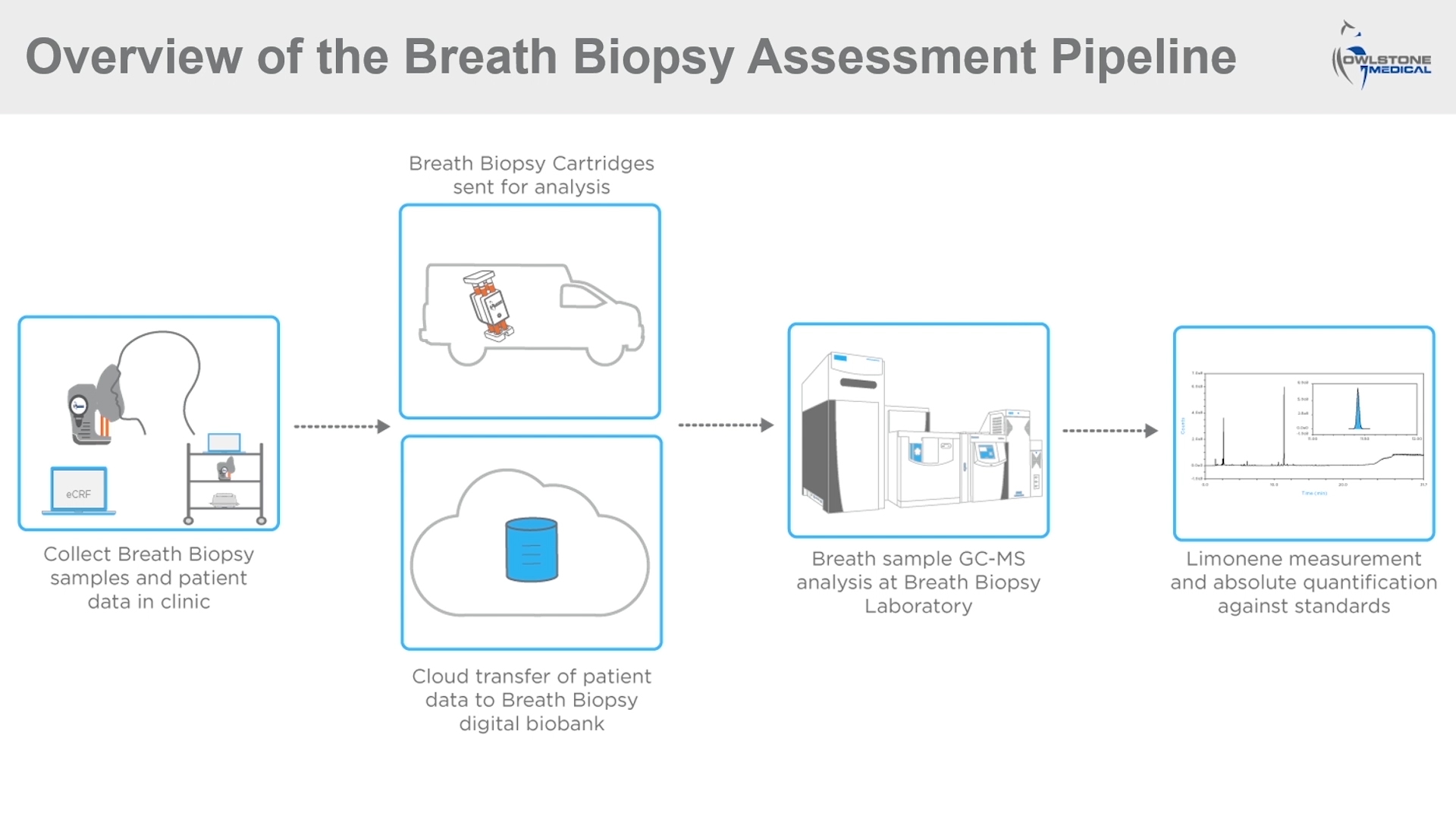
Figure 1. A slide from Dr. Ferrandino’s presentation that demonstrates the experimental method, using Breath Biopsy, for his investigation linking levels of breath limonene to liver disease
Dr Ferrandino went on to share unpublished results from the untargeted analysis of the same breath samples seeking to identify further breath biomarkers to complement limonene.
View Dr. Ferrandino’s paper Read our Case Study of this work
Speaking second, Dr Plevris, who has spent 10-15 years’ researching volatile organic compounds (VOCs) for disease across a range of diseases, discussed using breath volatiles to accurately and non-invasively stratify patients with NAFLD. He contrasted the use of GC-MS analysis and eNose technologies (gas sensor arrays that measure VOCs as a composite, rather than detect them individually).
A number of studies have focused on cirrhosis and managed to produce good results based on only a small number of samples. Comparatively fewer studies have looked at NAFLD and NASH though a number of biomarkers have been suggested, such as tridecane, 3-methyl-butanonitrile, 1 propanol. Plevris presented on a recent publication, Sinha et al., that used VOCs to stratify NAFLD. Applying GC-MS technology via a commercial lab, they used a semi-targeted, non-quantitative approach focusing on 19 VOCs from previous literature. Of these 19 molecules they found 7 to be of interest, of which 3 showed reliable prediction power (limonene, dimethyl sulfide and acetone). Limonene and dimethyl sulfide were able to generate a model with 98% area under the receiver operating characteristics (AUROC) for control vs. cirrhosis and 91% AUROC for NAFLD vs. cirrhosis.
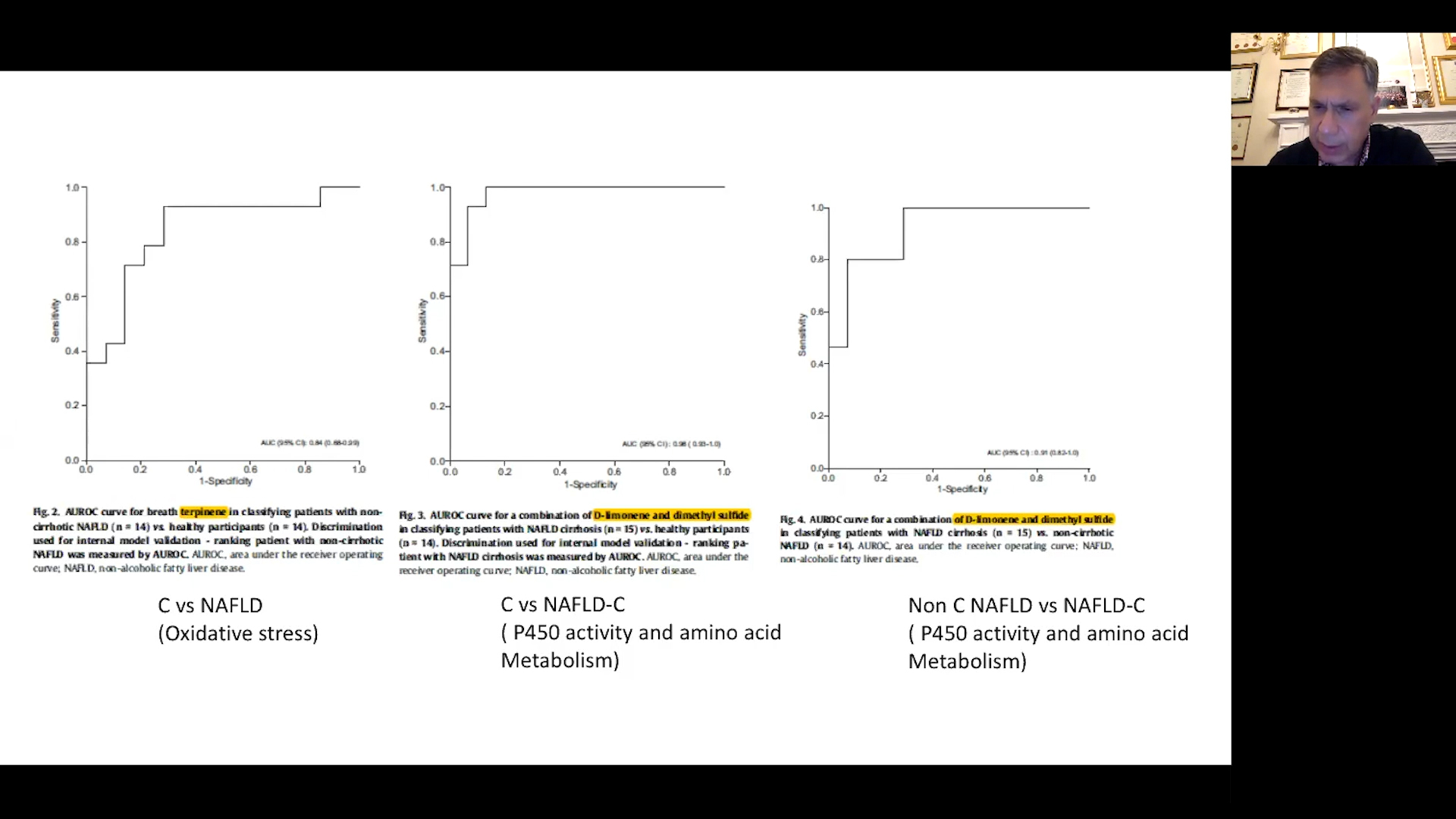
Plevris also discussed a similar study that had instead employed eNose technology. Breathprints were collected from 3 groups of 30 patients. The eNose allowed separation of cirrhosis from controls but produced no clear separation of NAFLD and cirrhosis, with the data being challenging to interpret due to a lack of biological insight. Dr Plevris concluded that eNoses may still be useful for NAFLD detection but require customization to target relevant volatiles based on biological understanding.
Dr Friedman concluded the liver session, discussing the current diagnostic challenges in NAFLD. While presenting several available measures of liver health, he highlighted liver fibrosis as the clearest indicator of patient outcomes. Fibrosis is caused by a wide range of conditions including NASH. Non-invasive methods for measuring fibrosis would allow the detection and monitoring of NAFLD progression.
Many current methods for diagnosing liver disease are, he said, overly dependent on age as a diagnostic factor and the quality of results deteriorates in older patients. Liquid biopsy of circulating nucleotides has demonstrated the potential for less direct diagnostic methods but has yet to show clear clinical results.
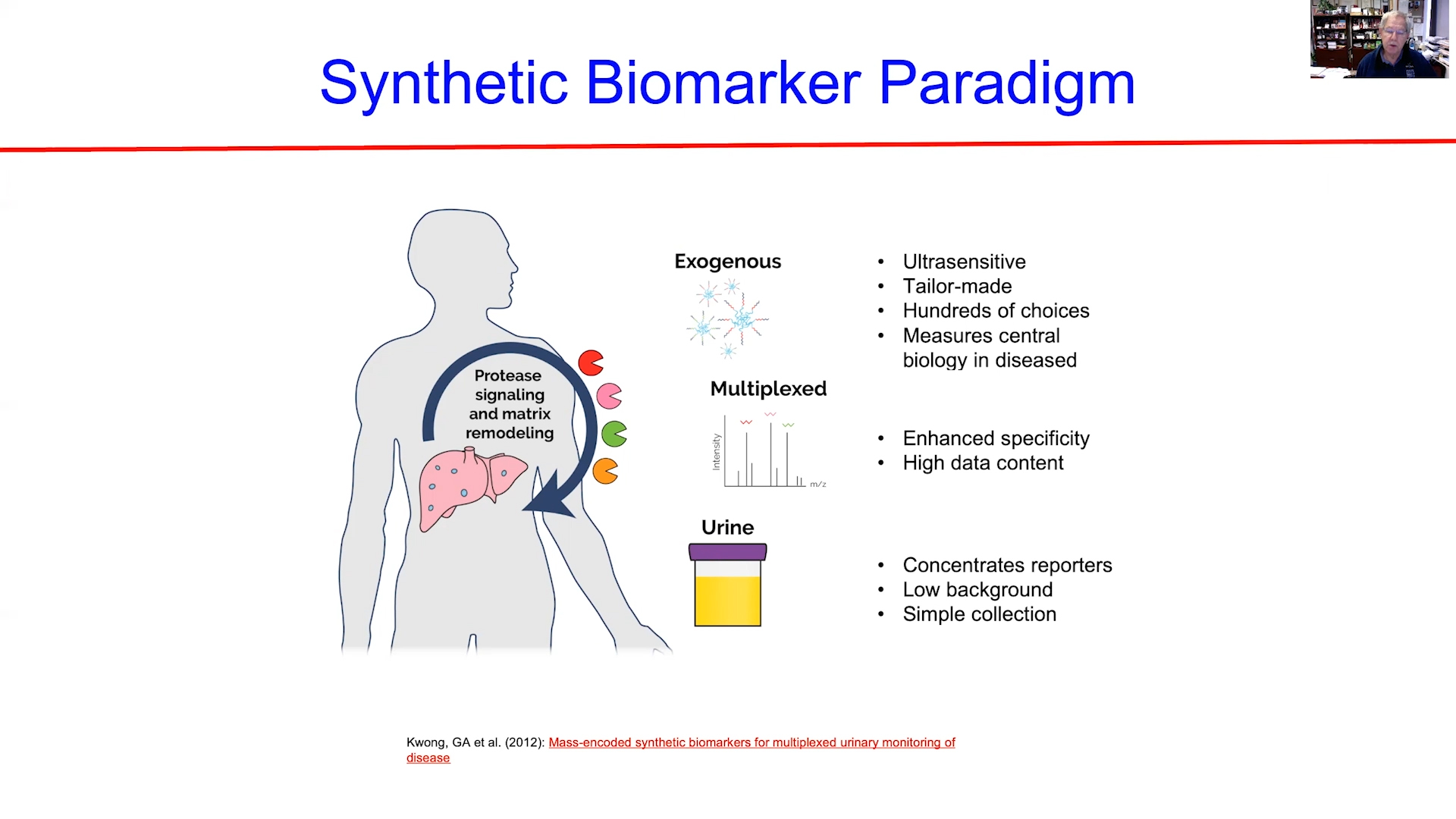
Dr Friedman finished his presentation discussing the role of proteases in NASH. He postulated that it might be possible to use administered peptides to probe the activity of these proteases which can then be detected non-invasively – a similar concept to using limonene as a probe, as suggested by Dr Ferrandino. Dr Friedman suggested that we may see breath tests for liver disease in the clinic within the next 5-7 years. It will be fascinating to see whether one of these approaches is the first to make that jump.
If you weren’t able to attend the Breath Biopsy Conference 2020 live, or you want to see any of the presentations again, don’t worry. The whole conference, including the liver session, is now available for you to watch on demand, for free. The next Breath Biopsy Conference will be at the Hilton Cambridge City Center (Cambridge, UK) on 12–13 October 2021. If you would like to join us, please express your interest now and we will be in touch when registration opens.
Watch online now Express Interest for 2021
