Volatile biomarkers
Volatile Biomarkers
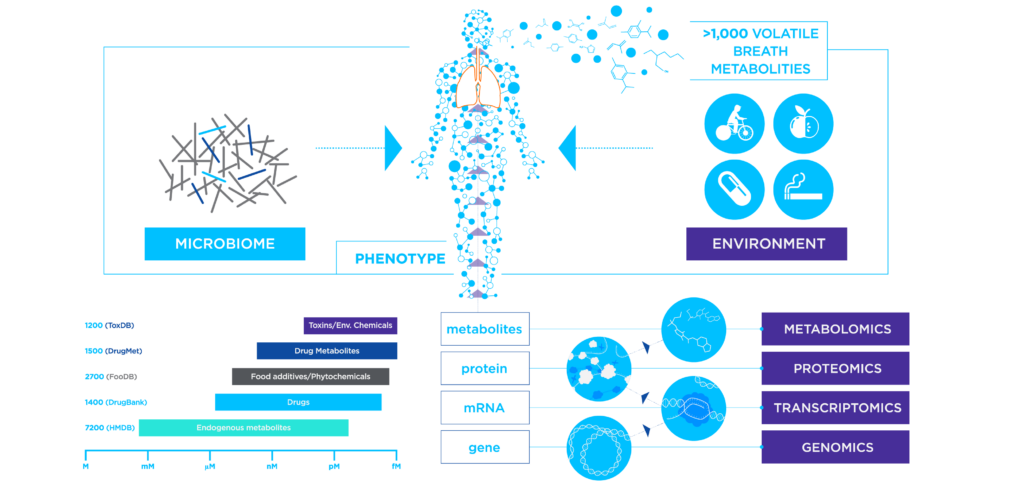
Bodily fluids such as blood contain cells, proteins, lipids, and metabolites that can be measured as biomarkers to inform on underlying physiological processes for various clinical purposes. Volatile organic compounds (VOCs) are gaseous molecules that can originate either from human metabolic processes within the body (endogenous VOCs) or from external sources such as diet, prescription drugs, microbial metabolism, and environmental exposure (exogenous VOCs). VOCs can be sampled quickly and non-invasively from breath with Breath Biopsy®, and are becoming increasingly studied throughout the medical field for their potential to act as useful biomarkers. The molecular weight of VOCs can vary significantly, ranging from very low (e.g., less than 50 g/mol) to high (e.g., several hundred g/mol). Generally, lower molecular weight VOCs tend to be more volatile, while higher molecular weight VOCs have lower volatility.
Studies have identified over 1,000 VOCs that can be found on breath, alongside respiratory droplets. A VOC (in medical terminology) can therefore provide a rich source of information regarding overall health and have great potential as VOC biomarkers: indicators of disease onset and progression.
Uses of breath biomarkers
Uses of Breath Biomarkers
Due to the unique properties of breath as a sampling medium, and the chemical attributes of VOCs, breath VOC biomarkers have many advantageous attributes for clinical, and research use. These include:
- Breath can be collected in a completely non-invasive manner, is pain-free, and is convenient for subjects providing samples, thus avoiding the disruption of a patient’s body.
- Breath can be collected serially at frequent intervals allowing for analysis of a time course after drug or dietary intervention.
- Breath is available in an unlimited supply, therefore a large volume of breath can be collected to pre-concentrate lower abundance metabolites for subsequent analysis.
- VOCs are a new range of molecules related to metabolic processes (including microbial metabolism related to the microbiome) to explore where other approaches may have failed.
- As large volumes of breath can collected, this can be concentrated to detect even very low-abundance VOCs.
- Volatile biomarkers have the potential to be deployed in point-of-care or even home-based settings for diagnosis and ongoing monitoring, our OMED Health Breath Analyzer is an example.
Breath Biopsy provides the means for non-invasive VOC analysis and detection produced by the metabolome with relevance to a wide range of diseases, including respiratory diseases, liver diseases, and cancers. The applications of Breath Biopsy span early detection, precision medicine, and environmental research with specific utility in treatment efficacy and safety monitoring during drug development.
ORIGINS OF VOCS
Origins of VOCs
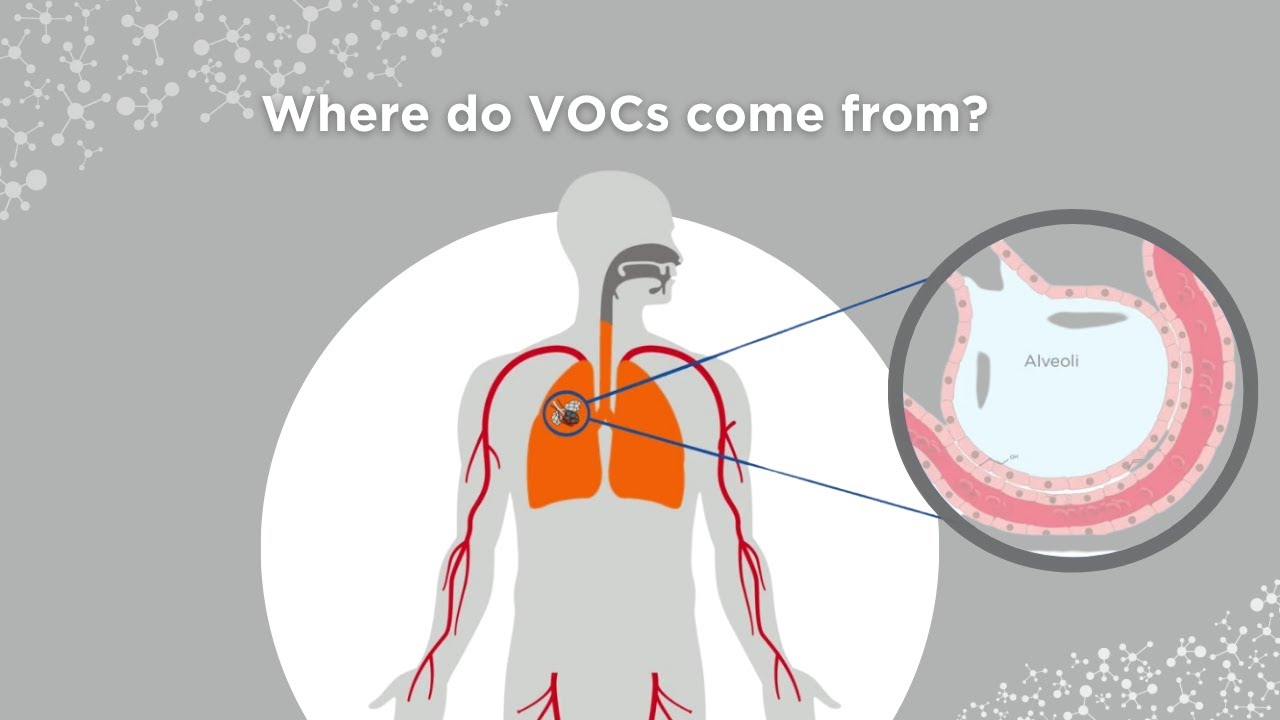
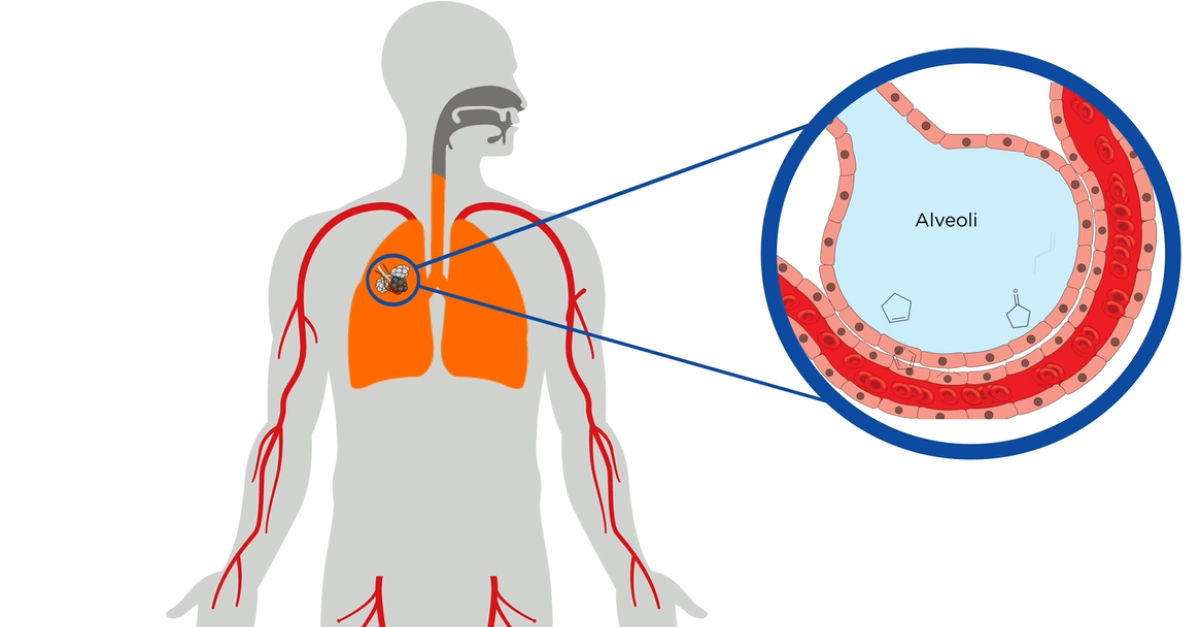
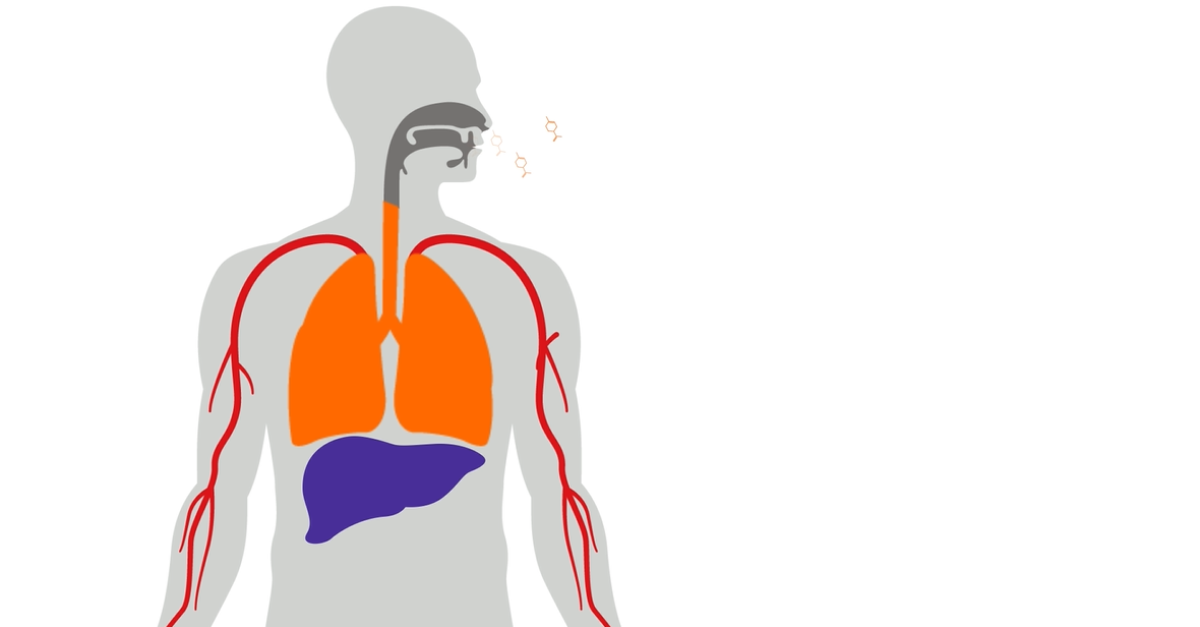
Endogenous volatile organic compounds are produced throughout the body and are picked up and distributed in the bloodstream. From the blood, they exchange into air in the lungs and are then exhaled along with respiratory droplets and atmospheric gases. Exhaled VOCs contribute to biomarker discovery by providing a source of useful biomarkers with clear associations to the body’s metabolism.
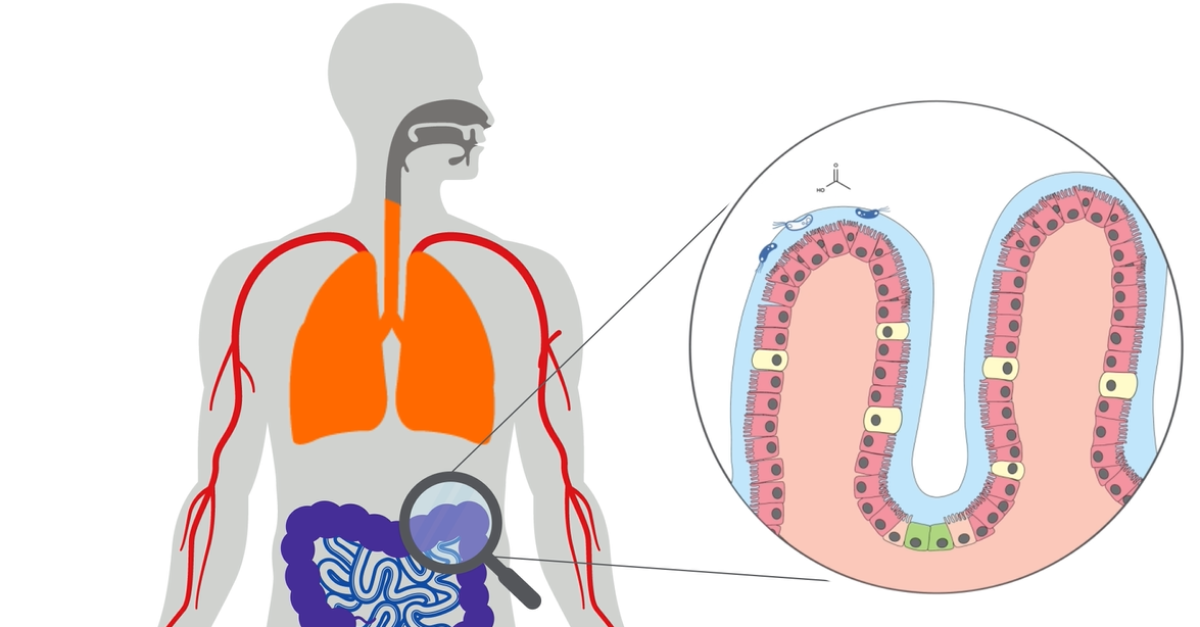
Exogenous volatile organic compounds have a broader range of origins and have largely been overlooked as environmental contaminants in biological samples. More recently, however, exogenous VOCs have become of increasing interest as many interact with biological systems and so can also provide valuable information relevant to health and disease. For example, exogenous VOCs produced from the gut microbiome can be key health indicators.
In order to better understand the composition of human breath, both in terms of understanding the diversity present in a healthy population, and the differences in different disease states, we have developed the Breath Biopsy VOC Atlas. This is a catalog of identified and quantified volatile organic compounds (VOCs) found in exhaled breath.
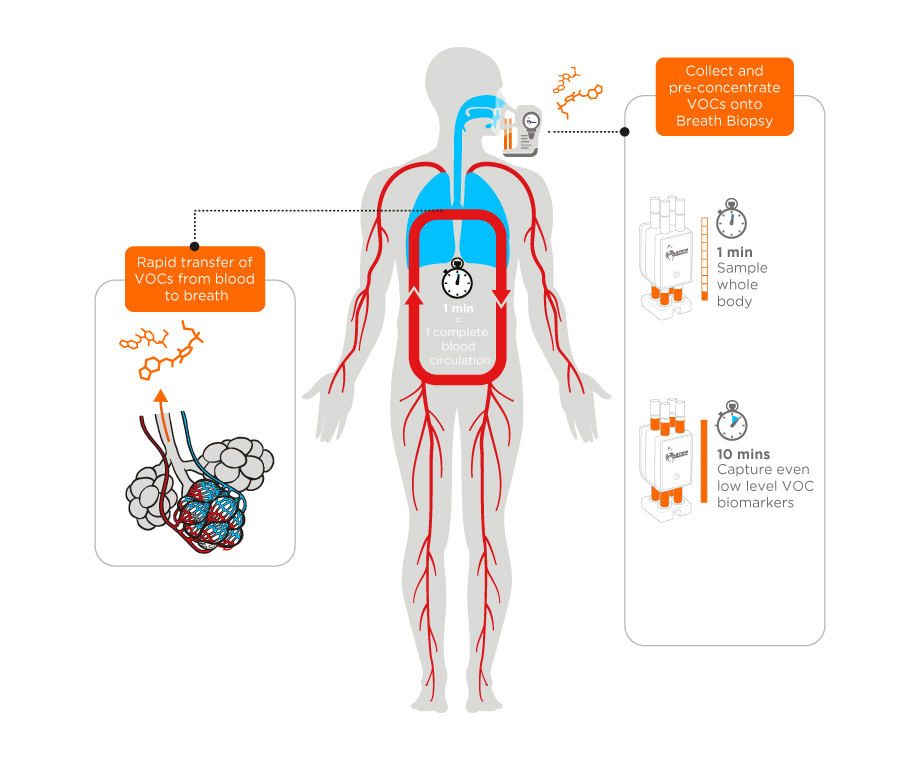
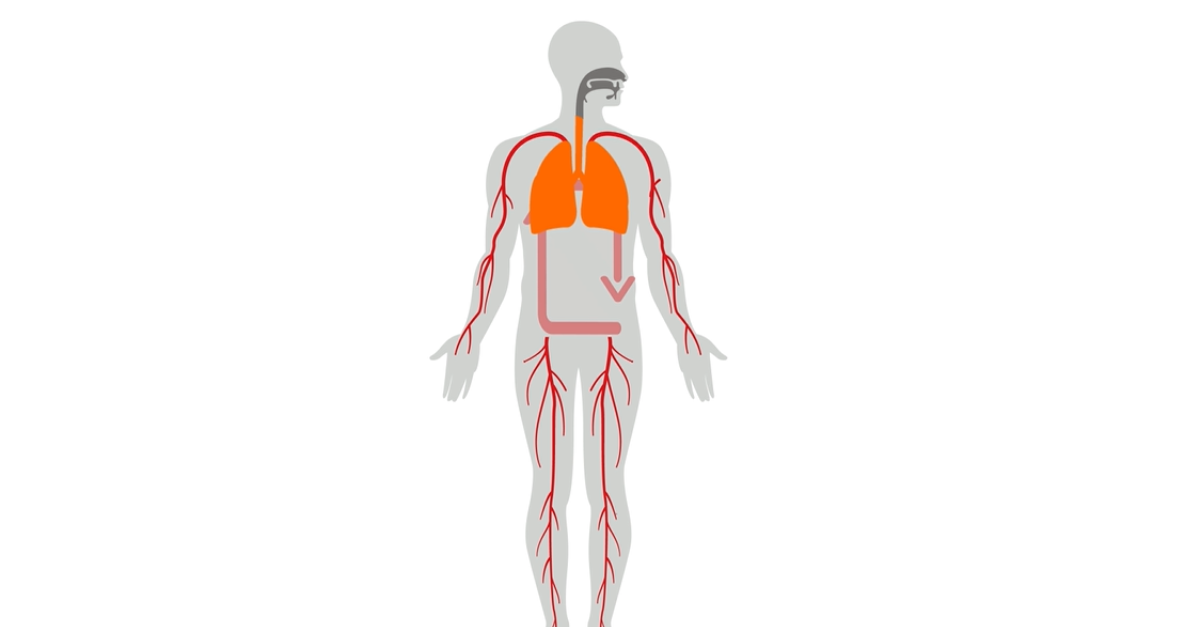
- Your lungs are very effective at exchanging chemicals with your blood, including VOCs that are generated throughout the body.
- It takes ~1 minute for your blood volume to circle around your body once.
- By continuously preconcentrating exhaled breath the entire circulating blood volume can be analyzed.
Targeted VOC probes
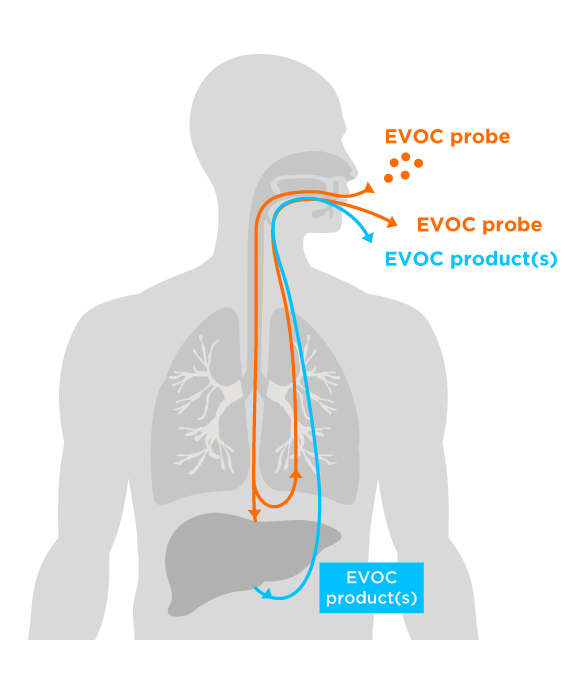
We have further harnessed the power of exogenous VOCs as EVOC Probes. Many exogenous VOCs are processed within the body by core metabolic pathways, which are also often involved in drug metabolism. By administering EVOC Probes, we can assess the activity of these pathways, which may be relevant in treatment selection and precision medicine. We are in the process of developing a range of breath tests that utilize EVOC probes, including one for the early detection of lung cancer.
FURTHER READING
Recommended Further Reading
Breath Analysis & Infectious Disease 101
Breath Analysis & the Respiratory System 101
Breath Analysis & the Liver 101
Breath Analysis & the Microbiome 101
- EBOOK: Breath Biopsy: The Complete Guide
- BLOG: 7 Reasons to Collect Breath Samples
- DIGEST: Breath Analysis with Breath Biopsy
- WEBINAR: An EVOC Probe for Fatty Liver Disease
- BLOG: Linking VOCs to Disease Biology
- WEBINAR: Identifying Translational Biomarkers using Breath Biopsy in vitro Headspace Analysis
- BLOG: Oxidative Stress and Lipid Peroxidation as a source of VOCs
- WEBINAR: Non-invasive Functional Assessment of the Microbiome from Exhaled Breath