Examining candidate breath biomarkers for kidney disease
Published on: 30 Aug 2022
Kidney disease, though common, is often diagnosed by routine blood or urine tests that a patient is undergoing for a different reason. Development of a non-invasive breath test could allow for cheaper screening and earlier intervention, when damage is less severe and treatment simpler. Recent studies have proposed a number of potential breath biomarkers that warrant further investigation.
Chronic kidney disease (CKD), is characterized by a gradual deterioration of kidney function over time. A loss of kidney function leads to increased levels of waste products in the blood, increasing the risk of other cardiovascular diseases and causing high blood pressure, anemia, nerve damage and even weakened bones. Around 37 million adults in the USA have CKD with a further 1 in 3 Americans at increased risk of developing the condition.1 Heart disease is the primary cause of death for people with CKD.
Early detection is key to preventing or delaying the progression of kidney disease to kidney failure, with lifestyle changes often being the most effective treatments, while the disease is still reversible. Unfortunately, the early stages of kidney disease normally pass undetected.
Why breath?
Breath sampling and breath analysis are attractive alternatives to currently available biomarker tests in many disease areas, for both diagnosis and ongoing monitoring, because it is completely non-invasive, convenient, and pain-free. Exhaled breath is an inexhaustible resource and providing a breath sample has been found acceptable even by patients reporting acute breathlessness.2
For thousands of years ‘fishy’ smelling breath and urine have been associated with renal disorders. VOCs (volatile organic compounds) produced throughout the body are picked up and distributed in the bloodstream before exchanging into air in the lungs. As kidney function deteriorates, it is logical to expect that some of the excess waste products left in the blood may be VOCs that can be detected on exhaled breath.
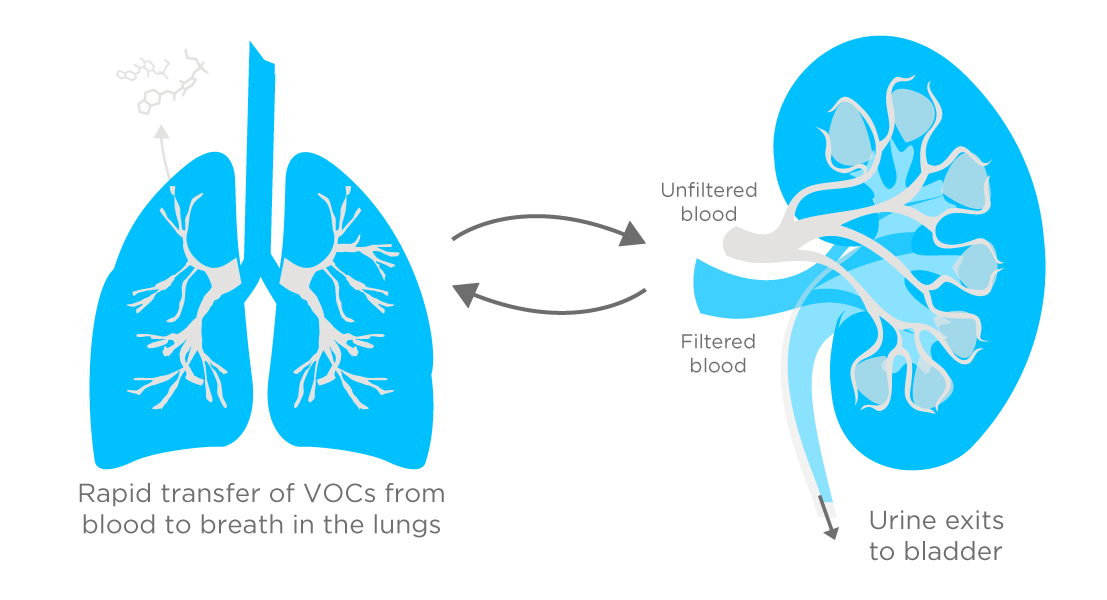
The compounds responsible for the ‘fishy smell’ are now known to be amines, but human breath contains a wide range of other VOCs which could prove to be useful biomarkers for kidney function. A number of recent studies have attempted to investigate the potential clinical value of these VOCs.
Candidate biomarkers
Trimethylamine
Trimethylamine (TMA) is one of the amines that is particularly responsible for the fishy-smelling breath associated with kidney disorders. Healthy individuals metabolize TMA in the kidneys, forming urea and formaldehyde. Impaired kidney function allows TMA to build up in the bloodstream over time, before being excreted, unmetabolized, on both breath and urine.
This strong link means that in the past TMA in blood plasma has been suggested as a kidney disease biomarker. However, blood sampling is invasive and burdensome, so Grabowska-Polanowska et al. investigated whether measuring TMA on breath could be a better option.3,4 Across two related studies they found TMA on the breath of CKD subjects but not present on the breath of healthy individuals. Other studies, such as Romani et al.’s work, have also adjudged TMA as a potential biomarker for CKD.5 Further work is needed to validate an association between TMA levels and disease severity and identify a TMA cutoff value that could be used for diagnosing CKD.
TMA is an exogenous VOC (EVOC) that is present in foods such as fish and normally ingested as part of a normal diet. This presents an opportunity for a study to investigate the use of TMA as an EVOC® Probe, in the same way that, at Owlstone Medical, we have explored the utility of limonene (a chemical in orange juice) as an EVOC Probe for liver disease.
Ammonia
The gut microbiota metabolizes proteins, creating a number of waste nitrogen compounds, with ammonia being one of the most common. As with TMA, ammonia can build up in the bloodstream when not being removed through healthy kidney function. In the study of more than 120 participants conducted by Romani et al. they found breath Ammonia to be the VOC that most accurately differentiated CKD patients from controls (AUC 0.902).5
This association is further supported by Obermeier et al.’s work with pediatric CKD patients.6 Importantly, their study found ammonia to be significantly elevated in patients with kidney disease relative to controls, including in patients with early-stage disease.
Dimethyl sulfide
Romani et al.’s study found dimethyl sulfide to be moderately accurate in predicting disease status (AUC 0.740), though Obermeier et al found that patients and controls exhaled similar amounts of dimethyl sulfide.5,6 A possible confounding factor is that organosulfur compounds have been noted to increase as a consequence of a subject’s age or concomitant conditions (such as diabetes), not simply CKD status.
Additional classes of VOCs have been tentatively associated with CKD, including amines, alkanes, aldehydes, and alcohols. Further work is required to elucidate the biological associations between VOC marker classes and validate VOC signatures of CKD that can be reliably translated into clinical care.
How can we help you?
The compounds discussed above may also be found in our Breath Biopsy VOC Atlas® – a comprehensive database of the identified and quantified VOCs found in exhaled breath. The Atlas also provides insight and scientific context to identified compounds to enable the confident selection of candidate biomarkers for a variety of diseases, including kidney disease. You can sign up for the Atlas here.
As interdisciplinary specialists in breath, we have created Breath Biopsy® OMNI to be the most advanced solution for reliable global breath biomarker analysis. And, when you choose to work with us, your investigation is further supported by our extensive study design, management, and data interpretation expertise.
Our Breath Biopsy Collection Station has been developed to maximize your chances of discovering robust breath biomarkers by ensuring optimal sample collection. The ReCIVA® Breath Sampler and CASPER® Portable Air Supply have both been specifically designed to increase signal-to-noise in breath samples (previously a significant challenge), and collect standardized samples that ensure high comparability between patients, even over multiple sampling locations and longitudinal time courses.
Developing a clinically useful test requires the identification of the VOCs that can be linked to underlying biology and the specific disease of interest. Breath Biopsy OMNI uses TD-GC-MS with high resolution and high dynamic range, maximizing the number of VOCs that can be studied in your breath sample.
Find out more about Breath Biopsy OMNI Let’s Talk
References
- Chronic Kidney Disease in the United States, 2021 https://www.cdc.gov/kidney-disease/php/data-research/?CDC_AAref_Val=https://www.cdc.gov/kidneydisease/publications-resources/ckd-national-facts.html
- Holden KA, Ibrahim W, Salman D, et al. (2020) Use of the ReCIVA device in breath sampling of patients with acute breathlessness: a feasibility study, ERJ Open Res. DOI: 10.1183/23120541.00119-2020
- Grabowska-Polanowska et al. (2013) Detection of potential chronic kidney disease markers in breath using gas chromatography with mass-spectral detection coupled with thermal desorption method J Chromatogr A. 2; 1301:179-89. DOI: 10.1016/j.chroma.2013.05.012
- Grabowska-Polanowska et al. (2017) The application of chromatographic breath analysis in the search of volatile biomarkers of chronic kidney disease and coexisting type 2 diabetes mellitus Journal of Chromatography B 1060 (2017) 103–110. DOI: 10.1016/j.jchromb.2017.05.030
- Romani et al. (2022) Utility of SIFT-MS to evaluate volatile organic compounds in nephropathic patients’ breath Sci Rep 12, 10413 (2022). DOI: 10.1038/s41598-022-14152-7
- Obermeier et al. (2017) Exhaled volatile substances mirror clinical conditions in pediatric chronic kidney disease PLoS ONE 12(6): e0178745. DOI: 10.1371/journalpone.0178745
Catch up on the presentations from the Breath Biopsy Conference 2024
