Insights into VOC biomarkers of diabetes
Published on: 22 Feb 2022
Diabetics globally rely on regular unpleasant and invasive blood tests to monitor their blood glucose levels – with mistakes having dangerous consequences. If we could replace the reliance on blood sampling with non-invasive breath, it could revolutionize both initial diagnosis and day-to-day life for millions of patients. Recent studies have shown this reality may not be as far away as you think.
Around the world an estimated 537 million people have diabetes, which encompasses a group of metabolic conditions characterized by high blood sugar levels over a prolonged period.1 Patients are commonly diagnosed via one of a number of blood tests.2 Providing a blood sample is invasive which, coupled with the diagnostic tests’ relative expense, seriously limits their applicability for widespread screening. Once diagnosed, regular checking of a patient’s blood glucose levels, via blood sample, is currently also key to ongoing monitoring. These methods, while accurate, are painful, invasive and inconvenient.
Why breath?
Breath analysis could offer an attractive alternative to currently available diabetes tests, for both diagnosis and ongoing monitoring since it is completely non-invasive, convenient, and pain-free.
Providing a breath sample requires no medical training and has been found to be acceptable even by patients reporting acute breathlessness.3 As a sampling medium this makes it uniquely appropriate for home use.
Using breath samples to diagnose diabetes, as one part of a complementary diagnostic process, is not a new idea. When someone who is diabetic experiences an absence of sufficient insulin to metabolize glucose, their body can instead begin burning fatty acids, producing an excess of acidic ketones. This process is called ketoacidosis and, amongst many other dangerous and debilitating symptoms, has also long been associated with strong and fruity-smelling breath. This is because acetone, one of the ketones produced, is exhaled in the breath. The exact relationship between acetone and diabetes has been investigated since as early as the 1940s.4
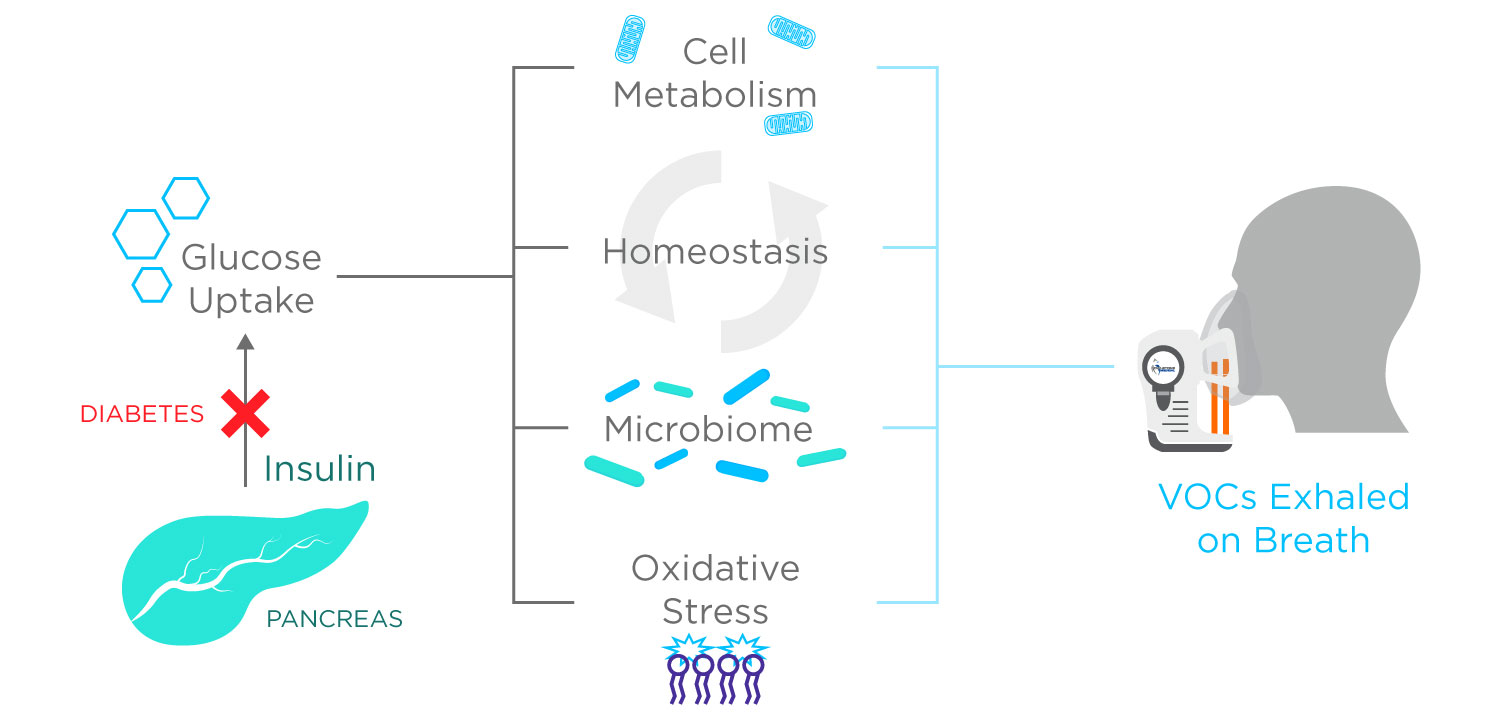
Alongside acetone, human exhaled breath contains a wide range of other volatile organic compounds (VOCs) which can be collected, detected and measured. VOCs may be generated endogenously in the body as either metabolic by-products of human cell processes or colonizing micro-organisms. VOCs can also be inhaled as exogenous compounds from the environment.
Endogenous VOCs produced in metabolic activity from all around the body are transported in the bloodstream and then exchanged into exhaled breath in the lungs. Identifying a breath biomarker that’s closely tied to blood-glucose levels, or the body’s mechanisms for metabolizing glucose, has the potential to both ease initial diagnosis and ongoing monitoring of diabetes – and consequently improve quality of life for hundreds of millions of people around the globe.
Potential biomarkers
While no breath-based biomarkers have yet been successfully validated for use with diabetes, studies have tentatively identified a number of candidate VOCs5, worthy of further exploration, which could have applications in this area:
Isotope-labelled 13CO2
A simple test based on the CO2 composition of exhaled breath was found to be effective by one study in discriminating subgroups.5 When participants ingested labelled glucose, identifying labelled CO2 on breath provided an insight into the rates of oxidation of glucose within the body. Unfortunately, labelled compounds are logistically tricky to produce at scale and then store, and the general public are also cautious about their use. So, while these results are extremely promising, labelled CO2 is unlikely to be suitable as a long-term option for mass screening.
Indole
In a recent study, Fink et al. undertook an untargeted search for potential biomarkers that correlate with blood glucose levels.6 They found that Indole showed a significant mean correlation to blood glucose levels across different diabetes types. Indole is known to be produced by bacteria digesting food in the gut, yet this doesn’t seem to be relevant here, meaning the source of indole in diabetes remains unknown. Future studies will need to validate its potential as a biomarker in diverse cohorts and investigate its actual relation to metabolic pathways.
Acetone
We’ve already mentioned acetone’s longtime association with diabetes in this blog. It’s created in the body through the decarboxylation of acetoacetate. The production of acetoacetate is influenced by alterations in fatty acid and/or glucose oxidation associated with diabetes. A meta-analysis of recent studies found acetone to demonstrate moderate diagnostic accuracy but limited sensitivity.5
A paper by Platonov et al (2024) developed a method for the rapid detection of acetone in exhaled breath using a mobile diagnostic complex based on microfluidic systems. Improving the detection of acetone in exhaled breath facilitates the diagnosis of changes in blood glucose levels, promotes early diabetes diagnosis, and supports the monitoring of therapeutic effectiveness.7
Isopropanol
A number of studies have found isopropanol to be at consistently higher levels on the breath of diabetics.5 Used as a diagnostic tool it’s been found to have moderate accuracy, with higher specificity than sensitivity. Unfortunately, it’s hasn’t been clearly linked to a specific metabolic pathway and could arise from several different enzymatic and/or non-enzymatic processes.
Dimethyl sulfide
A VOC particularly associated with the intestinal microbiome (likely reporting on shifts in microbiome composition associated with insulin resistance), it is not known to be produced by any mammalian metabolic pathways but instead is likely a product of bacteria living in the gut. There appears to be some variance in response to environmental effects (e.g. antibiotic use, day-to-day variation in diet) that may limit the suitability of this compound as a potential diagnostic marker.5
Read a case study on biomarkers of insulin resistance
How can we help you?
As interdisciplinary specialists in breath, we have created Breath Biopsy® OMNI to be the most advanced solution for reliable global breath biomarker testing. And, when you choose to work with us, your investigation is further supported by our extensive study design, management and data interpretation expertise.
Our Breath Biopsy® Collection Station has been developed to maximize your chances of discovering robust breath biomarkers by ensuring optimal sample collection. The ReCIVA® Breath Sampler and CASPER® Portable Air Supply have both been specifically designed to increase signal-to-noise in breath samples (previously a significant challenge), and collect standardized samples that ensure high comparability between patients, even over longitudinal time courses.
Developing a clinically useful test requires the identification of the VOCs that can be linked to underlying biology and the specific disease of interest. Breath Biopsy OMNI uses TD-GC-MS with high resolution and high dynamic range, maximizing the number of VOCs that can be studied in your breath sample.
Find out more about Breath Biopsy OMNI Let’s talk
Footnotes
- IDF Diabetes Atlas. Accessed February 2022. diabetesatlas.org
- American Diabetes Association (2009) Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 32:S62–S67. DOI: 10.2337/dc09-S062
- Holden K. A. et al. (2020) Use of the ReCIVA device in breath sampling of patients with acute breathlessness: a feasibility study. ERJ Open Res 6: 00119-2020. DOI: 10.1183/23120541.00119-2020
- A.P. Briggs et al. (1940) The management of diabetes as controlled by tests of acetone in expired air. The Journal of Laboratory and Clinical Medicine 25:6, p603-609. DOI: 10.5555/uri:pii:S0022214340904802
- Wang W. et al. (2021) Accuracy of breath test for diabetes mellitus diagnosis: a systematic review and meta-analysis. BMJ Open Diabetes Research and Care 9:e002174. DOI: 10.1136/bmjdrc-2021-002174
- Fink H. et al (2022) Indole as a new tentative marker in exhaled breath for non-invasive blood glucose monitoring of diabetic subjects. J. Breath Res. 16:026001 DOI: 10.1088/1752-7163/ac4610
- Platonov I. et al (2024) Rapid Detection of Acetone in Exhaled Breath for the Diagnosis of Diabetes Mellitus. Journal of Analytical Chemistry. Volume 79, pages 1856–1864. DOI: 10.1134/S1061934824701430
Catch up on the presentations from the Breath Biopsy Conference 2024
