Using exhaled methane to diagnose intestinal methanogen overgrowth
Single methane measurement shows promise as a new diagnostic method
| Publication information: W. Takakura et al. A Single Fasting Exhaled Methane Level Correlates With Fecal Methanogen Load, Clinical Symptoms and Accurately Detects Intestinal Methanogen Overgrowth Am J Gastroenterol 2022; 00:1–8. DOI: 10.14309/ajg.0000000000001607
Disease Area: Gastrointestinal Application: Diagnostics, treatment monitoring Sample medium: Breath, feces Summary:
|
Intestinal methanogen overgrowth (IMO) is a gastrointestinal condition associated with bloating, gas, abdominal discomfort and constipation, symptoms which can be alleviated with appropriate treatment. Currently IMO is diagnosed via breath testing over a two-hour window, taking advantage of the benefits of breath for high frequency repeat sampling. However, this time commitment can still be difficult for some patients, particularly if repeat tests are required as part of ongoing monitoring, post-diagnosis. If sampling duration could be reduced it could further add to the benefits of breath tests for both patients and healthcare providers.
In this recent breath study, Takakura et al. assessed the feasibility of using a single methane measurement (SMM) accompanied by fasting for both diagnosis and treatment monitoring of patients with IMO. Compared to small intestinal bacterial overgrowth, patients with IMO seem to have relatively stable methane levels on breath, so methane may be able to operate as a simple biomarker of disease, even within a single sample.
Results
To enable them to explore their hypothesis Takakura et al. had access to extensive historical data, including more than 12,000 lactulose breath tests and more than 700 glucose breath tests, taking a single methane measurement from these standard two-hour tests proved to be extremely effective. This data was from 3 different cohorts, collected at 2 different centers. Considering several different cut-off points (Methane between 2–10ppm in a single breath), the SMM diagnosis of IMO correlated with the lactulose test results with a sensitivity of between 86.4% and 98.8%, and a specificity of 99.3% to 100%. With the same cut-offs compared against the two-hour glucose test, the SMM performed with 86.4% to 98.8% sensitivity and 81.0% to 100% specificity.
To investigate the utility of methane as a biomarker for IMO, Takakura et al. considered how constant the breath methane measurement remained in patients who were diagnosed with IMO but went untreated. To do this, they compared SMM from the day of a 2-hour breath test with another SMM taken 14 days later and found very little change. Diagnosis of IMO on the basis of the 14 days measurements alone would have resulted in very similar sensitivity to that reported using the data from the test day above. Specificity couldn’t be assessed, as all patients providing SMM on day 14 were confirmed to have IMO. Further data from a placebo group in a treatment trial suggested SMM remained stable for at least 84 days. Once antibiotic therapies were introduced to treat IMO, SMM was found to significantly decrease over time.
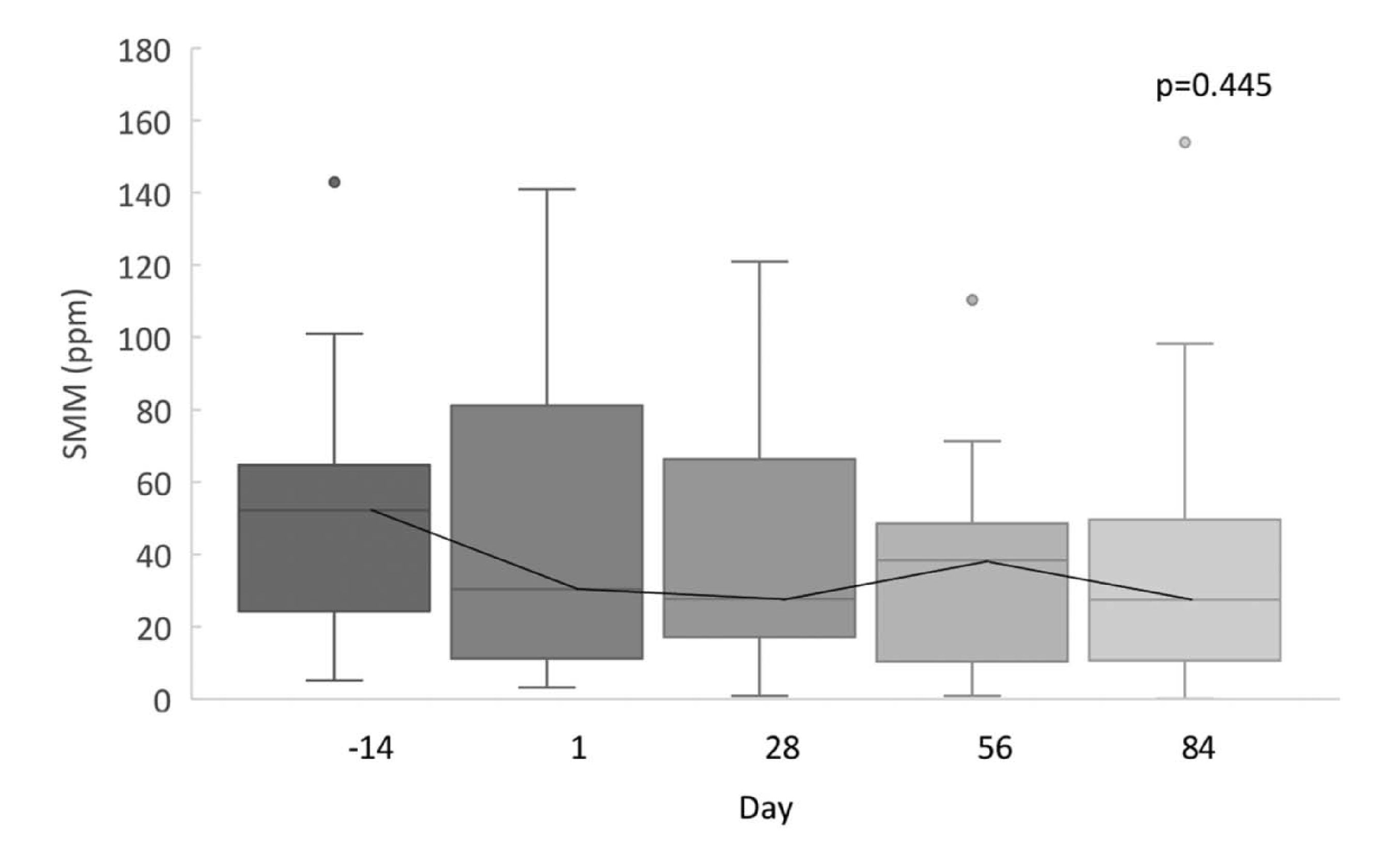
Figure 1: For subjects who received placebo, SMM did not change over time (n = 20).
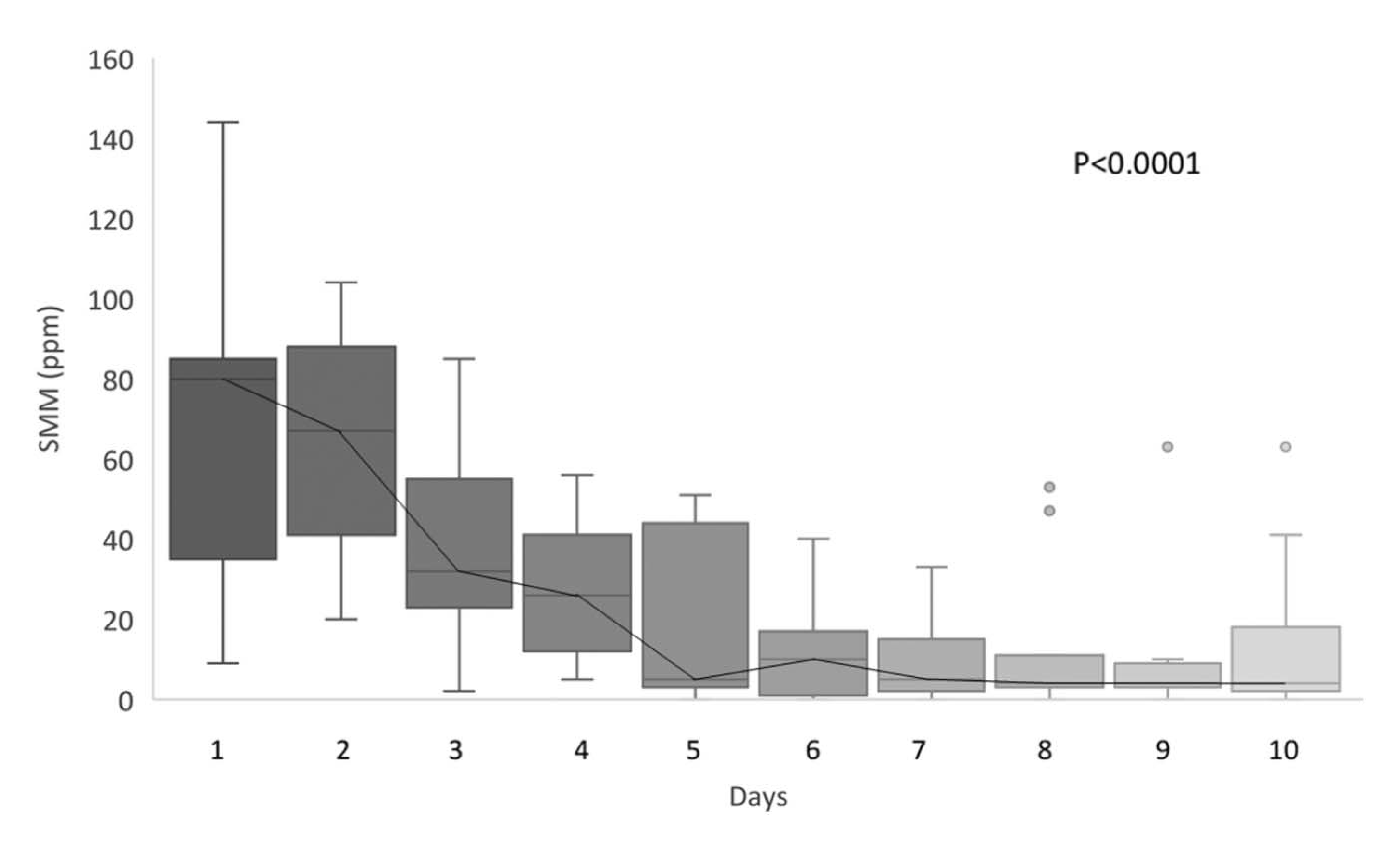
Figure 2: Daily SMM levels rapidly and significantly drop during antibiotic therapy. SMM, single CH4 measurement.
The SMM of each patient was found to be related to gastrointestinal symptoms: patients with an SMM greater than 10 ppm more likely to complain of constipation and patients under 10 ppm more likely to report diarrhea. Methane has been shown to slow intestinal motility, and the most abundant methanogen in the human gut is Methanobrevibacter smithii. Stool sequencing for M. smithii is another established diagnostic for IMO. Here, the SMM was also shown to correlate well with M. smithii concentrations on stool samples.
The strength of Takakura et al.’s results mean they feel confident concluding that SMM can accurately and non-invasively diagnose IMO, both as part of, and separate to, existing more cumbersome 2-hour breath tests. If, as it appears, the full breath test can be avoided, then this would cut down costs while increasing convenience for patients. Although larger trials are needed, their results also suggest that SMM could be used as a ‘simple and inexpensive tool to monitor treatment response in patients with IMO’ able to confirm either eradication or lack of eradication of IMO in the patient’s gut.
‘SMM shows promise as an inexpensive, noninvasive biomarker for intestinal methanogen load.’
Owlstone Medical has partnered with Functional Gut Diagnostics (FGD) to investigate novel biomarkers for gastrointestinal diseases like IMO and we are already able to offer similar at home breath tests for food intolerances and small intestinal bacterial overgrowth (SIBO).
We are currently working with FGD to investigate the impact of Iron on gut health and there is extensive research evidence to support the use of breath-based biomarkers with other common gastrointestinal diseases, like gastro-oesophageal reflux, IBD and IBS. You can find out more about the potential of breath tests to revolutionize gastrointestinal healthcare on our blog or by watching our webinar which is available on-demand.
