Breath Biomarkers a Priority for Asthma Diagnosis and Monitoring
Published on: 15 Feb 2018
Currently the diagnosis of asthma is based on clinical history, physical examination and lung function. However, these methods do not allow asthma to be diagnosed directly or to differentiate between phenotypes. It is recognized that there is a growing need for new diagnostic tools that relay the increasing understanding of different asthma phenotypes to objective tests.
This in time may lead to a shift from the traditional approach of treatment guided by symptoms towards the development of personalized medicine based on the exact underlying cause of asthma, and solve the current problems of over and under-diagnosis, over and under-treatment, and reduce asthma morbidity and mortality.
Key Priorities for Asthma Diagnostics in the Future
The European Asthma Research and Innovation Partnership (EARIP) aims to reduce asthma deaths in Europe by 25% within ten years and by 50% within 20 years. A recent paper by Garcia-Marcos entitled Priorities for future research into asthma diagnostic tools: A PAN-EU consensus exercise from the European asthma research innovation partnership (EARIP)1 reviews current asthma diagnostic tools and predicts the future direction of state-of-the-art technologies. The aim of the review is to identify opportunities for future investment of methods which allow the accurate diagnosis of different phenotypes of asthma.
The three developments considered most important are:
- Tools to measure volatile organic compounds (VOCs) in exhaled breath
- Prediction of future asthma in preschool children with reasonable accuracy
- New biological markers of asthma in genomics, proteomics and metabolomics as a tool for both diagnosis and monitoring
Biomarkers in Exhaled Breath
Evaluating the use of exhaled breath, the article delves into the history of using user-friendly biomarkers such as FENO. Garcia-Marcos notes that early attempts of using FENO to diagnose and monitor asthma suffered from unexpected setbacks. Whilst it was initially thought that FENO was a general marker of asthma on closer inspection it was found that FENO mainly reflects eosinophilic airways inflammation.
The use of biomarkers is recognized as a promising but underexplored area and the section on VOCs in breath finishes remarking:
Further exploring the value of VOCs to assist phenotyping asthma and predicting major clinical outcomes such as exacerbations and response to treatment would be of great interest.
VOCs in the Metabolome
The general importance of VOCs is recognized by Garcia-Marcos when he discusses system biology, the field of study that focuses on the complex interaction within biological systems.
Asthma is a complex disease with many cell types being affected by diverse immunological pathways resulting in different phenotypes. Studying genomics, proteomics and metabolomics related to asthma offer great opportunities by allowing the assessment of several mediators simultaneously. This can lead to the discovery of early diagnostic profiles and can shed light on new biomarkers that may be applied to monitor asthma and to guide therapy.
Metabolomics is already being applied to asthma using a variety of biofluids, and the same approach is now being explored for volatile metabolites in exhaled breath. As mentioned by Garcia-Marcos, VOC biomarker profiles have been shown to to allow the differentiation between asthmatic and healthy children2.
Breath Biopsy
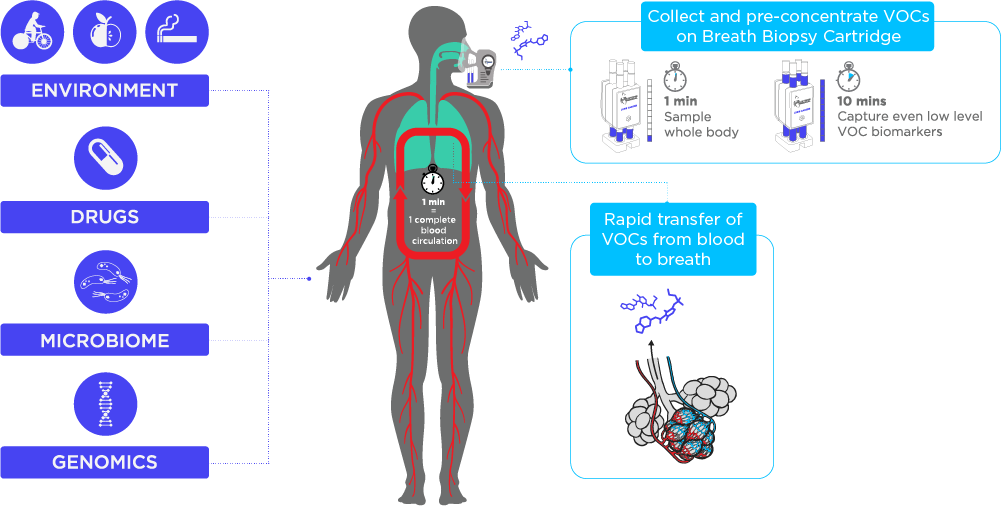
Volatile organic compounds in exhaled breath reflect metabolic processes taking place in the body, as well as its microbiome and environmental exposures. As VOCs in the bloodstream are efficiently exchanged with air in the lung’s alveoli, measuring VOCs in breath allows metabolic processes occurring throughout the body to be analyzed non-invasively.
The profile of VOCs in breath could provide a richer source of information compared to FENO as a single biomarker, and in trials VOCs have outperformed FENO in discriminating asthmatics vs. healthy controls3. Figure 1 outlines the potential applications for breath biomarkers in respiratory diseases, from disease phenotyping to patient stratification.
Further information about the measurement of VOCs in breath and the potential to discriminate between different asthma phenotypes and to aid identification of the correct asthma treatment can be found here:
References
1. Garcia-Marcos L, Edwards J, Kennington E, et al; the EARIP Collaboration. Priorities for future research into asthma diagnostic tools: A PAN-EU consensus exercise from the European asthma research innovation partnership (EARIP). Clin Exp Allergy. 2018;48:104–120. https://www.ncbi.nlm.nih.gov/pubmed/29290104
2. Dallinga JW, Robroeks CM, van Berkel JJ et al. Volatile organic compounds in exhaled breath as a diagnostic tool for asthma in children. Clin Exp Allergy 2010;40:68-76. https://www.ncbi.nlm.nih.gov/pubmed/19793086
3. Montuschi P, et al; Diagnostic performance of an electronic nose, fractional exhaled nitric oxide, and lung function testing in asthma. Chest. 2010 Apr;137(4):790-6. https://www.ncbi.nlm.nih.gov/pubmed/20081096
Breath Biopsy®
If you want to learn more about how Owlstone Medical’s Breath Sampling and Analysis technology is being investigated for uses in asthma why not check out our free ebook: Breath Biopsy: The Complete Guide?