
Integrate Breath Biopsy® into your COVID-19 Research
Exploring Breath Biomarkers for COVID-19 Research
The 2020 COVID-19 pandemic (also referred to as SARS-CoV-2 or Coronavirus) has had widespread impacts across the world. As an infection that primarily affects the lungs, the application of breath analysis could be an effective tool in managing COVID-19 infection and understanding its wider health impacts.
Owlstone Medical®‘s Breath Biopsy platform provides wide-ranging breath-based biomarker discovery capabilities that are available to address research challenges with relevance to COVID-19. These could include:
- Capture of viral particles or RNA in respiratory droplets using disposable breath collection devices and analysis using PCR or novel diagnostics.
- Non-invasive assessment and monitoring of lung damage resulting from COVID-19 infection using volatile organic compounds and other non-volatile macromolecules, such as inflammatory mediators, in exhaled breath. Discovery workflows may identify biomarkers to help stratify patients and optimise the use of ventilators and specialist care resources in the face of high demand.
- Investigating the relationship between COVID-19 and pre-existing conditions or environmental factors such as air pollution by measuring exogenous and endogenous volatile compounds on exhaled breath. The Breath Biopsy platform supports broad-ranging biomarker discovery as well as targeted panel analysis making it useful for investigating the impacts of various biological and environmental factors.
If you are interested in exploring applications for Breath Biopsy in your COVID-19 research, get in touch:
Using Biomarkers on Breath for Viral Infections
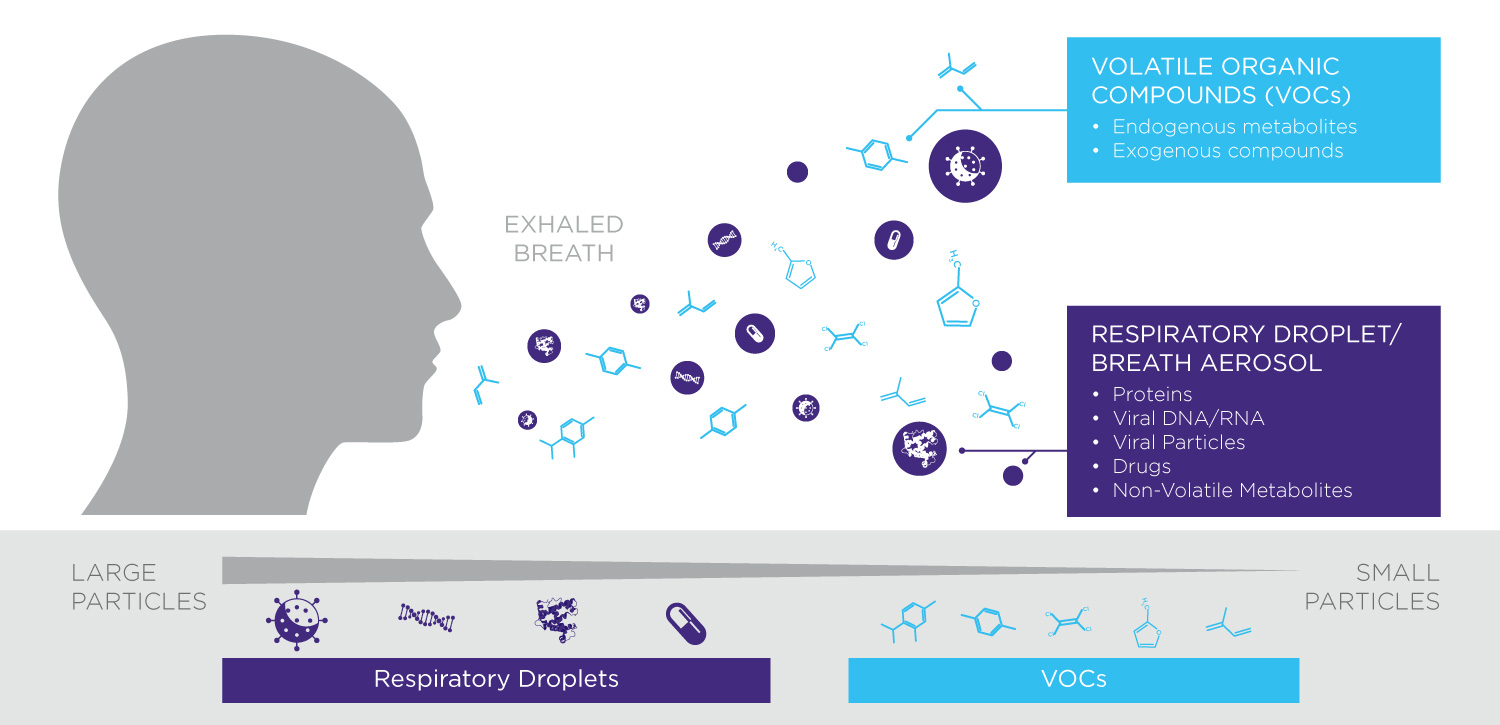
Beyond the gases in the air, exhaled breath is a rich source of potential biomarkers for use in a wide range of medical and health-related contexts. These can primarily be divided into volatile organic compounds (VOCs) and respiratory droplets. Many VOCs are produced as a result of metabolic processes throughout the body and reach the breath via the bloodstream, they can also originate in the airways or from exogenous sources such as air pollution. Respiratory droplets are produced from fluids within the lungs and airways and can carry proteins, nucleotides or even whole viruses and bacterial cells.
At Owlstone Medical we conducted an exhaled breath aerosol study investigating the feasibility of diagnosing COVID-19 using the viral load that’s deposited by patients on face mask filters.
This work revealed that breath testing was less sensitive for COVID-19 diagnosis than nasal swabs are, but it is possible that detecting viruses in breath aerosols could be developed as a means to assess risk of transmission. A paper discussing the results of our study was published in Nature’s journal: Scientific Reports. We have published a case study and a press releaser which gives a short overview of the key results and their relevance in context to the clinical need and other publications.
Selected research papers with relevance to using breath biomarkers to study COVID-19:
- Houspie et al. (2011) – Detecting respiratory viruses in exhaled breath condensate. DOI: 10.1186/1743-422X-8-98
- Anfinrud et al. (2020) – Visualizing the effect of face mask use on the release of exhaled breath aerosols. DOI: 10.1056/NEJMc2007800
- Yan et al. (2018) – Measurement of seasonal influenza viral particles and RNA from breath collected during normal breathing and coughing. DOI: 10.1073/pnas.1716561115
- Fabian et al. (2008) – Detecting influenza RNA in fine aerosols generated during regular tidal breathing. DOI: 10.1371/journal.pone.0002691
- Leung et al. (2020) – Surgical face masks help to prevent spread of respiratory viruses via respiratory droplets in exhaled breath. DOI: 10.5061/dryad.w9ghx3fkt
- Mitchell et al. (2016) – Detecting exhaled respiratory viruses on filters from spirometry devices. DOI: 10.1088/1752-7155/10/4/046002
- Milton et al. (2013) – Highest numbers of influenza particles detected in fine aerosols (<5μm) with use of surgical masks reducing the average number of detectable viruses by 3.4-fold. DOI: 10.1371/journal.ppat.1003205
- Zheng et al. (2020) – Meta-analysis of risk factors in COVID-19 severity and mortality. DOI: 10.1016/j.jinf.2020.04.021
- Leung et al. (2020) – Elevated ACE-2 expression in smokers and COPD patients may explain increased risk of COVID-19 infection. DOI: 10.1183/13993003.00688-2020
- Wu et al. (2020) – US-based study indicating that increased levels of particulate air pollution contribute to increased COVID-19 mortality. DOI: 10.1101/2020.04.05.20054502
- Cui et al. (2003) – Demonstrating a correlation between air pollution index and SARS fatalities. DOI: 10.1186/1476-069X-2-15

