Biomarkers for Gastrointestinal Diseases
Gastrointestinal diseases, such as inflammatory bowel disease (IBD), irritable bowel syndrome (IBS), small intestine bacterial overgrowth (SIBO), and colonic dysbiosis, together affect over a billion people worldwide. VOCs on breath have great potential as biomarkers for the detection of key disease mechanisms.
Published on: 25 Feb 2021
Gastrointestinal diseases, such as inflammatory bowel disease (IBD), irritable bowel syndrome (IBS), small intestine bacterial overgrowth (SIBO), and colonic dysbiosis, together affect over a billion people worldwide1. These conditions are characterized by shared non-specific symptoms including bloating, gas, pain, nausea, diarrhea and constipation, which can be mild or debilitating and often vary over time. Overall, gastrointestinal diseases and their effects in the US alone are estimated to cost over $21 billion per year2, including healthcare costs and lost productivity due to illness.
The common and non-specific symptoms of gastrointestinal diseases create a serious issue for clinicians and patients. Current tests are often invasive, expensive, time consuming, require specialist expertise, and can be causes of discomfort and distress for patients. These challenges combined with the embarrassing nature of these illnesses mean that it can take years for a patient to receive a satisfactory diagnosis and start effective treatment.
Introducing non-invasive biomarkers for gastrointestinal disease
An extensive and rapidly growing body of evidence suggests that volatile organic compounds (VOCs) have great potential as biomarkers with potential to become a valuable component of rapid and reliable differential diagnosis of gastrointestinal diseases. VOCs include a wide variety of small organic molecules that vaporize into the air at standard temperatures. They have a range of origins (including perfumes, paints, cleaning products, pollution etc.), yet some are the result of biological processes and are associated with key metabolic pathways, including respiration, and the digestion and absorption of food. Collecting and studying these VOCs can provide valuable insights into metabolic and disease processes.
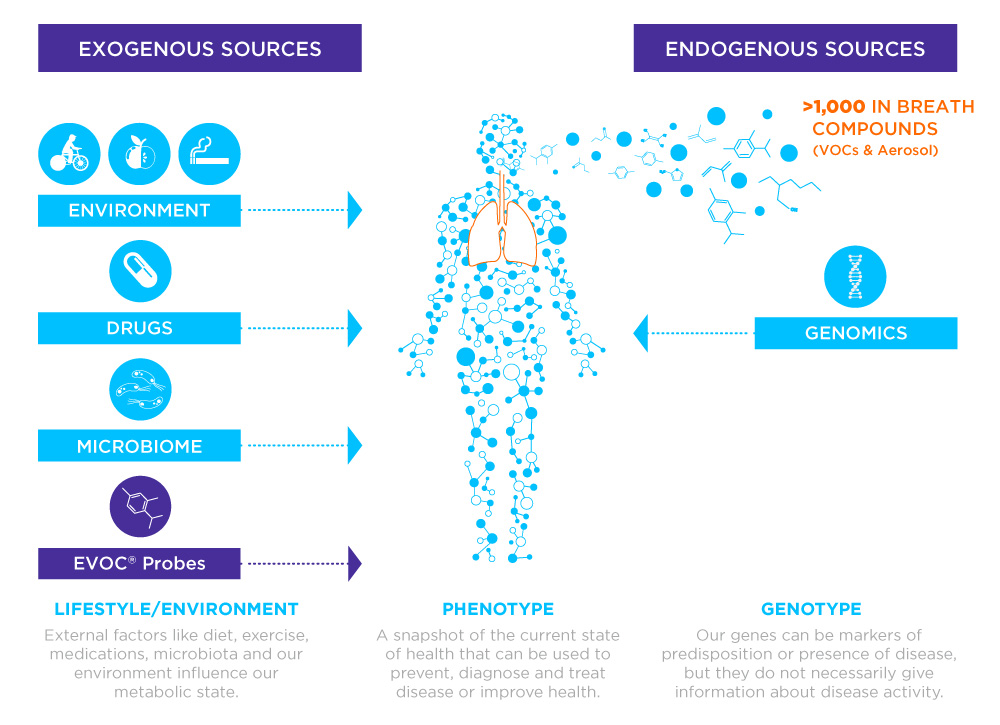
VOCs relevant to gastrointestinal diseases can be collected from various sources, including feces, urine and breath. Feces offers direct insights into processes within the gastrointestinal tract itself, particularly the lower bowels. Breath, however, can include VOCs absorbed into the blood from the gut, as well as from upper gastrointestinal sources, and systemic metabolites related to the body’s response to an illness. Over 1,000 different VOCs have been reported to be found on breath. Breath sampling is also largely preferable for patients and is suitable for frequent longitudinal sampling, where samples can be used to monitor how the body responds to a metabolic stimulus over time.
The benefits of VOC biomarkers for gastrointestinal diseases
In addition to the diversity of VOCs emitted from the human body, the non-invasive approaches to VOC collection, and the various ways that they can be associated with disease processes, there are a number of further benefits to using VOCs to study gastrointestinal diseases.
Similar tests are already in diagnostic use
Hydrogen methane breath tests (HMBT), are already in use to assess microbiome metabolism in certain gastrointestinal conditions, such as small intestine bacterial overgrowth (SIBO) and carbohydrate intolerances. HMBTs are available for diagnostic use by healthcare professionals in various countries, including the US and UK. While hydrogen and methane are not typically considered VOCs, their origins and the methods for collecting and analyzing them are all very similar.
There are clear connections between gastrointestinal processes and VOC production
The gut is highly metabolically active and it is to be expected that processes occurring in the gut, as well as downstream processes in the liver, will be diverse sources of VOCs. This is particularly apparent for microbiome metabolism within the gut itself. The microbiome benefits from access to distinct metabolic processes that are not present in other parts of the body, as such it produces uniquely identifiable compounds – including hydrogen and methane, as indicated above. There is great untapped potential to identify other VOC biomarkers associated with the rich diversity of life in the gastrointestinal tract.
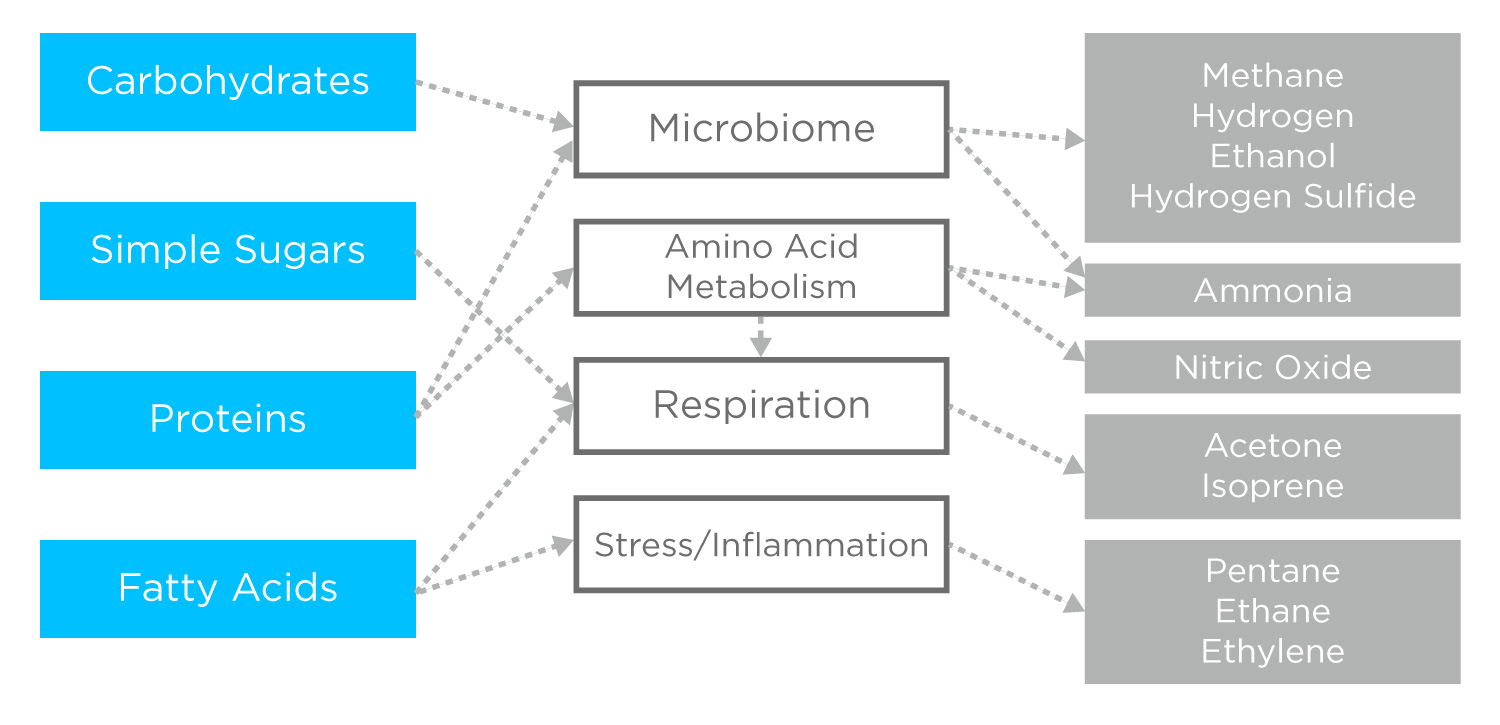
Gastrointestinal disease processes are associated with VOC production
Many gastrointestinal diseases are characterized by inflammation, which is associated with VOC production through processes such as oxidative stress and lipid peroxidation. While inflammation can occur in many settings, evidence suggests that the specific mechanisms of inflammation, and the resulting VOCs, can be context specific. Various Breath Biopsy® studies have already explored inflammation in other contexts, including the lungs, liver and cancer. As such, we’re well equipped for studies looking to examine inflammation in the gut and to investigate tissue-specific biomarkers of inflammation.
More about VOCs and lipid peroxidation
Significant evidence supports the use of VOCs as biomarkers for gastrointestinal diseases
The use of VOCs for tests with clinical relevance to early disease detection and precision medicine is under investigation across a range of disease contexts. There is a rapidly growing body of evidence to support the development of VOC tests for clinical use and many prospective biomarkers have been proposed. The development of Breath Biopsy is driven by the goal of providing robust, reliable biomarker analysis capabilities, to ensure reproducible biomarker discovery and validation that can enable rapid transition to clinical application.
If you are interested in finding out more about VOC biomarkers and how they can be integrated into research to better detect, diagnose and treat gastrointestinal diseases, get in touch with our team to arrange a conversation.
Our on-demand webinar with Dr Anthony Hobson is themed around breath biomarkers for gastrointestinal diseases and our next blog on this topic looks at existing research into gastrointestinal VOC biomarkers.
Watch the webinar READ THE BLOG
References
- Nirwan et al. (2020) Global Prevalence and Risk Factors of Gastro-oesophageal Reflux Disease (GORD): Systematic Review with Meta-analysis Sci. Rep. 10, 5814 DOI: 10.1038/s41598-020-62795-1
- https://www.aboutibs.org/facts-about-ibs/statistics.html
- Kurada et al (2015) Review article: breath analysis in inflammatory bowel diseases Aliment. Pharma. Therap. 41, 329-341 DOI: 10.1111/apt.13050
Catch up on the presentations from the Breath Biopsy Conference 2024

