FAIMS could help diagnose Bile Acid Diarrhea cheaply and quickly
Chronic diarrhea is estimated to affect up to 5% of the population.
| Publication information: J. A. Covington et al. Application of a Novel Tool for Diagnosing Bile Acid Diarrhoea, Sensors 2013, 13, 11899-11912; DOI: 10.3390/s130911899
Disease Area: Bile Acid Diarrhoea Application: Improved Diagnostics Sample medium: Urine Products: Lonestar® VOC Analyzer Analysis approach: Enose, FAIMS and GC-MS Summary:
|
Bile acid diarrhea (BAD) is a common form of chronic diarrhea caused by inadequate reabsorption of bile acid produced as part of the fat digestion process. Reabsorption can be perturbed through disease, surgical removal of a length of bowel or through defects in certain regulatory proteins. Diagnosis currently requires patients to swallow a capsule of radioactive selenium-75 tagged to homochlorotauric acid. The cost for this procedure (around £210 per patient) means that it may not be offered to patients in certain areas.
This study by Covington et al. has correlated cases of BAD with the presence of 2-propanol and acetamide in urine, and shown the potential for instant, non-invasive diagnosis using Owlstone Medical’s Lonestar VOC analyzer for urine sample analysis. Lonestar uses Owlstone Medical®‘s highly sensitive chip-based FAIMS technology. FAIMS spectra are information rich, and provide a wealth of useful compositional data for both researchers and clinicians.
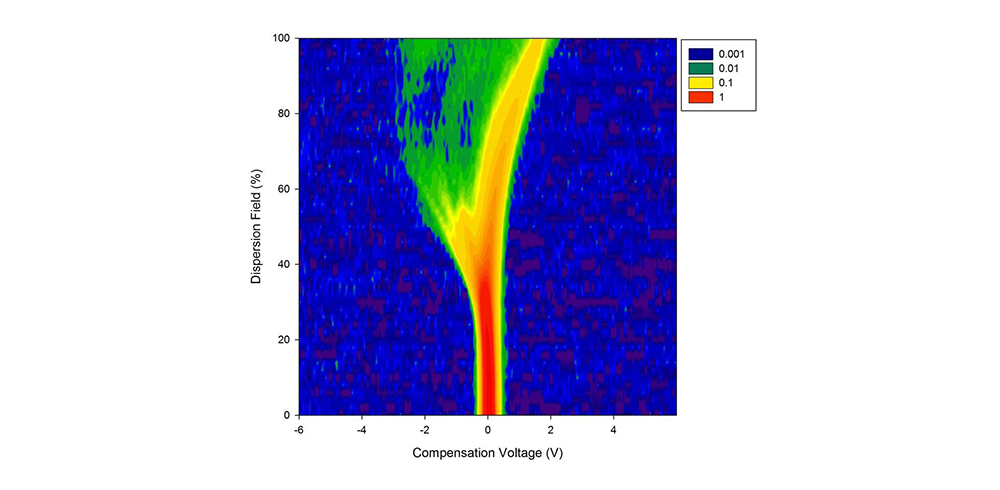
An example FAIMS spectra of a urine sample from a patient with bile acid diarrhea.
Gut bacteria play a key role in the cleavage of bile acids, but they are challenging to culture in the lab making studying them difficult. One approach to studying the role of gut bacteria in diseases such as bile acid diarrhea is analysis of the fermentation products they generate in the gut. Analysis of ‘the fermentome’ can be achieved through chemical analysis of the volatile chemical components given off by stool or urine samples. Detection of characteristic biomarkers in the fermentome using VOC analysis technology (such as FAIMS) would be much less invasive and cheaper than using radiological imaging for the diagnosis of conditions like bile acid diarrhea.
Using Linear Discriminant Analysis (LDA), the authors were able to successfully differentiate between patients with BAD, those with ulcerative colitis (which has very similar symptoms, but a very different underlying cause), and members of a control group.
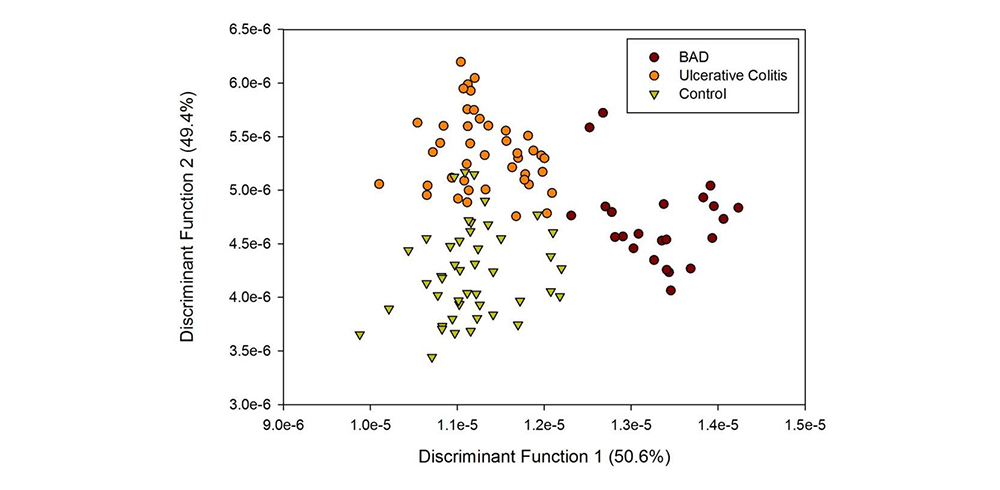
Linear discriminant analysis allows the detection of patients with bile acid diarrhea.
Differences in the FAIMS spectra of urine samples from patients with BAD, ulcerative colitis and controls could be the result of altered biodiversity of gut microflora, which cleave bile acids. GC-MS analysis of urine samples found that 2-propanol and acetamide were prominent only in patients with BAD. These compounds could therefore potentially be used to distinguish BAD from other disease groups.

