The Key to Early Detection – Mouth Cancer and Breath Analysis
Published on: 7 Nov 2023
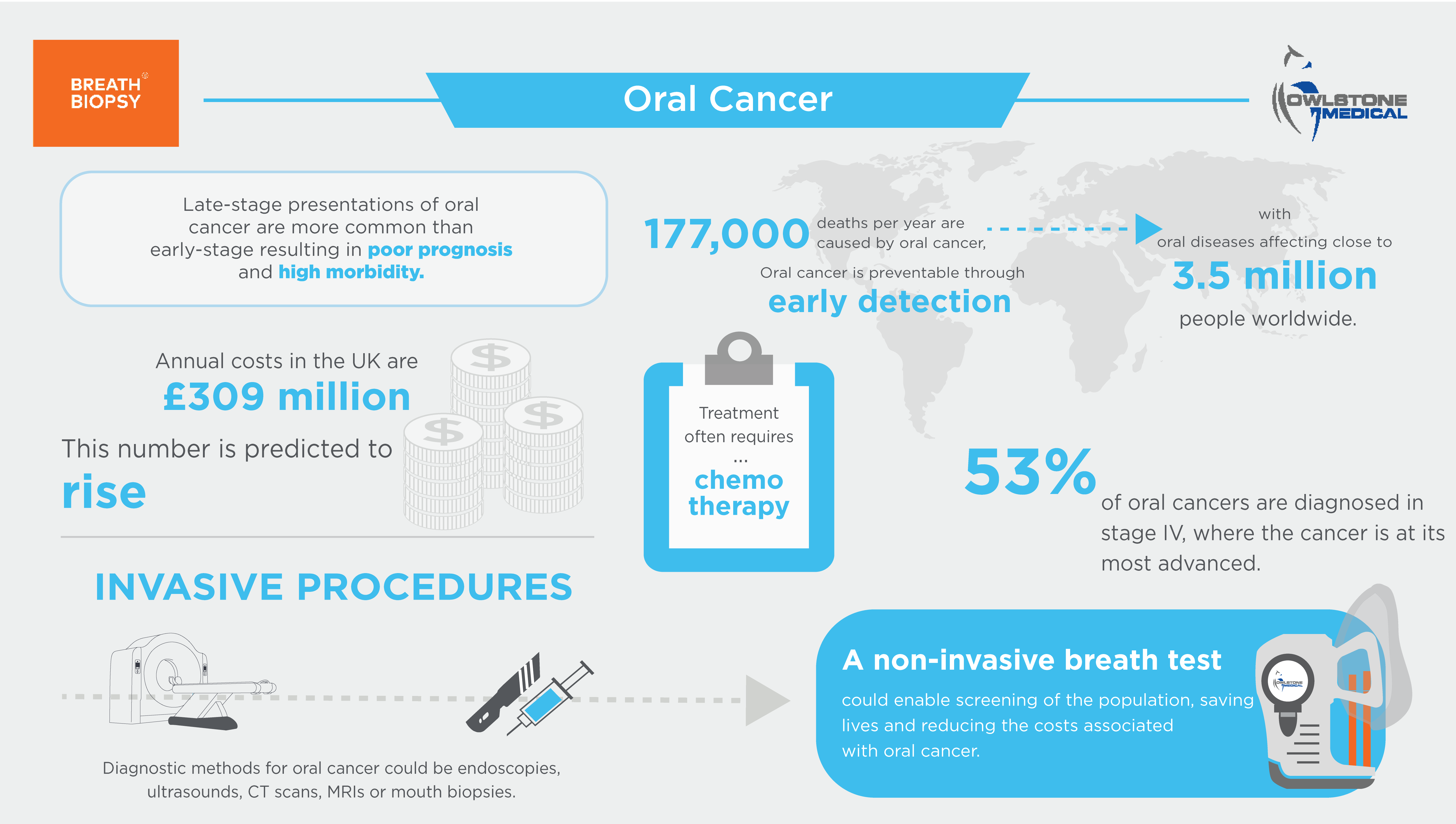
Oral cancer, specifically oral squamous cell carcinoma (OSCC), is a significant global health concern, ranking sixth in worldwide cancer prevalence, with OSCC accounting for a staggering 90% of all oral cancer diagnoses (1). The main causes of oral cancer worldwide are tobacco usage and the heavy consumption of alcohol, with statistics revealing that there are approximately 377,000 new cases of oral cancer annually, claiming the lives of 177,000 patients each year (1). This highlights the urgency of addressing oral cancer as it has a markedly high mortality rate when compared to other cancers.
Although the oral cavity (mouth) is easily accessible, oral cancer presents a challenging diagnostic landscape with up to 50% of oral cancer cases remaining undetected until the disease has advanced to the later stages (2). In its early stages, oral cancer is frequently asymptomatic, and its characteristics often mimic those of other oral diseases or benign tumors (3). Current therapies for oral cancer are effective when treating the early stages of the disease, however, late-stage presentations are more common and are often associated with poor prognosis and high treatment-related morbidity (4).
Furthermore, the nature of OSCC means that squamous cells can enter the lymphatic system, make their initial appearance in neck lymph nodes, and even spread to more distant sites such as the lungs (3). The complex and multifaceted nature of oral cancer draws attention to the pressing need for extensive research and improved diagnostic strategies to combat this disease. Early detection methods are needed to improve the treatment outcomes of oral cancer patients; analysis of exhaled breath could provide a non-invasive method to identify biomarkers in cancer and diagnose oral cancer early.
Compounds in breath that are associated with oral cancer.
Volatile organic compounds (VOCs) are found in various excreted biological materials and can serve as indicators of metabolic shifts triggered by oral cancer, including inflammation, necrosis, and degeneration. The metabolic by-products from these processes are released into the bloodstream and reach the alveoli, renal tubules, and gastrointestinal tract where they can be excreted in breath, urine, and feces (5). In oral cancer cases, these VOCs can be released directly into the breath as it is in constant contact with the oral cavity, and therefore VOCs are promising targets for new biomarkers for oral cancer screening and diagnosis.
Evidence for the potential of cancer detection through exhaled breath VOCs has gained support from recent studies using gas chromatography/mass spectrometry (GC-MS). These studies have unveiled distinct profiles of exhaled VOCs associated with various cancers including lung cancer (6), breast cancer (7), prostate cancer (8), and colorectal cancer (8). A study by Hakim et al. used GC-MS and Nanoscale Artificial Nose (NA-NOSE) to analyze breath from oral cancer patients and healthy controls.
The NA-NOSE could clearly distinguish between oral cancer patients and healthy controls and the GC-MS analysis found statistically significant differences in the breath composition between the two groups (9). The study found differences in the levels of 5 different VOCs in the breath between the two groups, including 4,6-Dimethyl-dodecane, 2,2-Dimethyl-propanoic acid, 5-Methyl-3-hexanone, 2,2-Dimethyl-decane, and limonene (9). We have already determined that Limonene can be used as a biomarker for liver disease (10) as it is absorbed and metabolized by enzymes in the liver, resulting in high levels of limonene found in the breath of cirrhotic patients when these enzymes are downregulated (11).
Methyl mercaptan, a volatile sulfur compound, is commonly detected in the oral cavity and has strong associations with periodontal disease and bad breath. It is worth noting that individuals with oral cancer often experience consistent bad breath (12), and therefore quantifying bad breath using methyl mercaptan as a biomarker could potentially help identify patients at a higher risk of oral cancer due to poor oral hygiene and bad breath.
The treatment and prevention of oral cancer have been hindered by the lack of knowledge of the disease and therefore more research must be dedicated to this significant public health concern. The identification and understanding of VOCs in breath as potential biomarkers for the early detection of oral cancer represents a promising avenue of research. Enhanced research efforts in this area hold the potential of earlier detection, improved treatment outcomes, and ultimately a reduction in the number of deaths caused by oral cancer worldwide.
Breath analysis can support oral cancer research.
VOCs that originate from oral cancer-specific metabolism can readily enter our oral cavity and be exhaled from the body in breath. These compounds can be analyzed in breath and can provide insight into the development and prognosis of oral cancer. As breath is a sampling medium that is in direct contact with the oral cavity, analysis of breath can provide a better insight into the disease as opposed to blood or urine which are more indirect. Breath is a virtually inexhaustible resource, with large volumes able to be collected at frequent intervals, meaning breath analysis can provide an almost real-time longitudinal analysis of VOCs.
The non-invasive nature of breath analysis makes it more attractive than tissue biopsies where damage can occur to the surrounding tissue and can be uncomfortable for the patient. This is especially relevant when we are speaking about mouth biopsies, where post-operative discomfort and bleeding are common side effects, and eating sticky, hard, brittle, spicy, and acidic food is often discouraged for the day following the procedure (13).
We are the world leaders in breath research for the early detection of disease, which is crucial in the fight against oral cancer. We are here to help you include breath analysis in your research. Breath Biopsy OMNI can provide everything you might need to start or continue using breath analysis, and you can receive expert advice from our team of scientists.
Through our Breath Biopsy Collect software used alongside our ReCIVA breath collection device, the specific fraction of breath collected can be customized based on your research focus. This flexibility can allow the selective capture of VOCs originating from the oral cavity. You can cross-check your data against our VOC Atlas to better understand how VOCs behave in a healthy population and confidentially validate your oral cancer biomarkers.
References.
- Tranby EP, Heaton LJ, Tomar SL, Kelly AL, Fager GL, Backley M, et al. Oral Cancer Prevalence, Mortality, and Costs in Medicaid and Commercial Insurance Claims Data. Cancer Epidemiol Biomarkers Prev. 2022 Sep 2;31(9):1849–57. DOI: 10.1158/1055-9965.EPI-22-0114
- Ford PJ, Farah CS. Early detection and diagnosis of oral cancer: Strategies for improvement. J Cancer Policy. 2013 Mar 1;1(1):e2–7. DOI: 10.1016/j.jcpo.2013.04.002
- Shigeyama H, Wang T, Ichinose M, Ansai T, Lee SW. Identification of volatile metabolites in human saliva from patients with oral squamous cell carcinoma via zeolite-based thin-film microextraction coupled with GC–MS. J Chromatogr B. 2019 Jan 1;1104:49–58. DOI: 10.1016/j.jchromb.2018.11.002
- Dharmawardana N, Goddard T, Woods C, Watson DI, Ooi EH, Yazbeck R. Development of a non-invasive exhaled breath test for the diagnosis of head and neck cancer. Br J Cancer. 2020 Dec;123(12):1775–81. DOI: 10.1038/s41416-020-01051-9
- Strimbu K, Tavel JA. What are Biomarkers? Curr Opin HIV AIDS. 2010 Nov;5(6):463–6. DOI: 10.1097/COH.0b013e32833ed177
- Fuchs P, Loeseken C, Schubert JK, Miekisch W. Breath gas aldehydes as biomarkers of lung cancer. Int J Cancer. 2010;126(11):2663–70. DOI: 10.1002/ijc.24970
- Shuster G, Gallimidi Z, Reiss AH, Dovgolevsky E, Billan S, Abdah-Bortnyak R, et al. Classification of breast cancer precursors through exhaled breath. Breast Cancer Res Treat. 2011 Apr 1;126(3):791–6. DOI: 10.1007/s10549-010-1317-x
- Peng G, Hakim M, Broza YY, Billan S, Abdah-Bortnyak R, Kuten A, et al. Detection of lung, breast, colorectal, and prostate cancers from exhaled breath using a single array of nanosensors. Br J Cancer. 2010 Aug;103(4):542–51. DOI: 10.1038/sj.bjc.6605810
- Hakim M, Billan S, Tisch U, Peng G, Dvrokind I, Marom O, et al. Diagnosis of head-and-neck cancer from exhaled breath. Br J Cancer. 2011 May;104(10):1649–55. DOI: 10.1038/bjc.2011.128
- Ferrandino G, Ricciardi F, Murgia A, Banda I, Manhota M, Ahmed Y, et al. Exogenous Volatile Organic Compound (EVOC®) Breath Testing Maximizes Classification Performance for Subjects with Cirrhosis and Reveals Signs of Portal Hypertension. Biomedicines. 2023 Nov;11(11):2957. DOI: 10.3390/biomedicines11112957
- Ferrandino G, Orf I, Smith R, Calcagno M, Thind AK, Debiram-Beecham I, et al. Breath Biopsy Assessment of Liver Disease Using an Exogenous Volatile Organic Compound—Toward Improved Detection of Liver Impairment. Clin Transl Gastroenterol. 2020 Sep 16;11(9):e00239. DOI: 10.14309/ctg.0000000000000239
- Szabó A, Tarnai Z, Berkovits C, Novák P, Mohácsi Á, Braunitzer G, et al. Volatile sulphur compound measurement with OralChromaTM: a methodological improvement. J Breath Res. 2015 Jan;9(1):016001. DOI: 10.1088/1752-7155/9/1/016001
- Biopsy Post-Operative Instructions Champaign IL. Available from: https://www.gumdoc.net/instructions-post-op-care/biopsy/
Catch up on the presentations from the Breath Biopsy Conference 2024