Breath biomarkers for cardiometabolic diseases
Published on: 28 Mar 2022
Significant and lasting metabolic changes contribute to, and are hallmarks of, cardiometabolic diseases such as diabetes, heart failure and chronic kidney and liver diseases. Non-invasive breath tests that reliably detect metabolism-linked biomarkers of cardiometabolic diseases would improve quality of life for patients and reduce the burden on healthcare systems by detecting more cases in the early stages and helping to predict acute events such as heart attacks or liver decompensation.
Cardiometabolic diseases and their risk factors
Cardiometabolic diseases are a collection of highly prevalent, often preventable illnesses that have become more common over recent decades and are typically associated with significant shifts in metabolic activity throughout the body. Several of the leading causes of death worldwide are cardiometabolic diseases, and in total they can be linked to around 20 million deaths per year [1]. Rises in deaths of working-age adults can also largely be attributed to these illnesses [2]. Additionally, treatment options are limited and typically require an organ transplant and early detection represents a vital alternative that gives patients time to make lifestyle changes to slow or avoid disease progression.

In addition to genetic and environmental components, key risk factors for cardiometabolic illness include smoking, lack of exercise, high fat/high sugar diet and high alcohol consumption, which have all contributed to the rapid increase in disease incidence that has been seen over the last 50 years. Obesity has been one of the most notable contributors and can increase the risks of complications during treatment. Since 1975, the number of obese people in the world has more than trebled and around 25% of people are now overweight or obese [3].
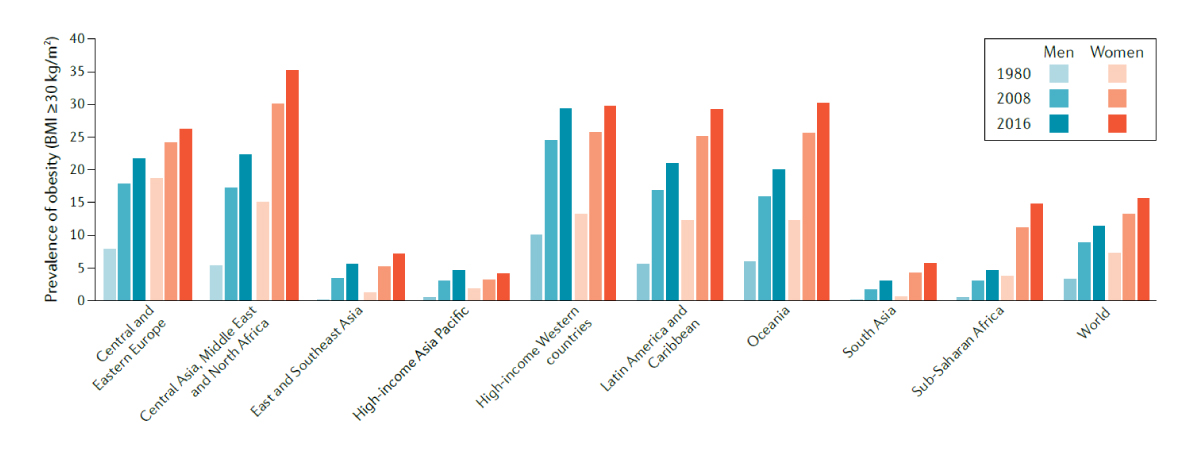
A fundamental metabolic change associated with cardiometabolic disease is a shift toward lipids as a source of energy rather than glucose, this is driven by factors such as mitochondrial dysfunction leading to shifts in lipid processing and storage. Additional changes have also been associated with these diseases such as endocrine signaling from adipose tissues, and alterations in the microbiome [5,6]. For example, Walker et al. demonstrated how reduced diversity in the microbiome can related to increased risk of obesity, cardiovascular disease and diabetes [7].
Our previous blogs further examine links between VOCs and chronic liver diseases and diabetes:
breath analysis for liver diseases breath analysis for diabetes
Cardiometabolism and VOCs on Breath
Some of the oldest examples of diagnostic breath testing relate to VOCs from cardiometabolic diseases. Hippocrates described fetor hepaticus a bad smell on breath associated with liver diseases and now known to be caused by dimethyl sulfide. Similarly, acetone from ketoacidosis leads to a fruity smell on the breath of diabetics, and dimethylamine and trimethylamine give a urine smell to the breath of people with uremia.
Metabolic pathways produce characteristic organic compounds which get released into the bloodstream. These include volatile organic compounds (VOCs) which can exchange out of the blood and into breath in the lungs. Since different metabolic processes produce different VOCs, changes to certain VOCs on breath can be expected to reflect altered cellular metabolism. Therefore, VOCs could be used to detect changes that are specific to different cardiometabolic diseases.
More recently, a small but growing number of breath research studies have looked to associate VOCs with cardiometabolic diseases. Reviews by Pereira et al. [8] and Cikach et al. [9] provide extensive summaries of VOCs that have been reported to associate with several cardiometabolic diseases. Examples include:
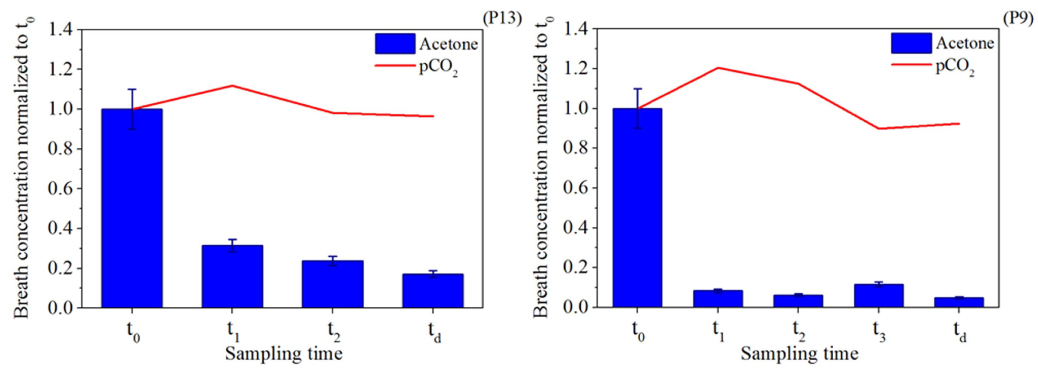
- Acetone, a product of lipid metabolism, reported in studies of diabetes and heart failure. May also be reduced in the body to 2-propanol. Acetone levels are high following acute heart failure and return slowly to normal levels over time [10].
- Pentane and ethane, end products of lipid peroxidation, a common metabolic process associated with reactive oxygen species, and involved in oxidative stress and inflammation [11]. Have been notably reported in studies of myocardial infarction and chronic heart failure. Alkanes and methylated alkanes have been linked to lipid peroxidation in a range of other contexts too including post-transplant allograft rejection [12].
- Nitric oxide (NO), a signaling molecule with roles including inflammation, immune responses and vasodilation that has also been linked to heart failure.
- Ethanol, a possible product of fermentation by the gut microbiome and relevant in a number of cardiometabolic diseases, however levels on breath are easily influenced by alcohol consumption.
- Limonene, our own work and that of others has consistently shown an increase in limonene on the breath of liver disease patients [13-17]. More recently, it was also reported by Khan et al. to be reduced in insulin resistant patients [18]. Click the buttons for more on these studied.
limonene in liver diseases limonene in insulin resistance
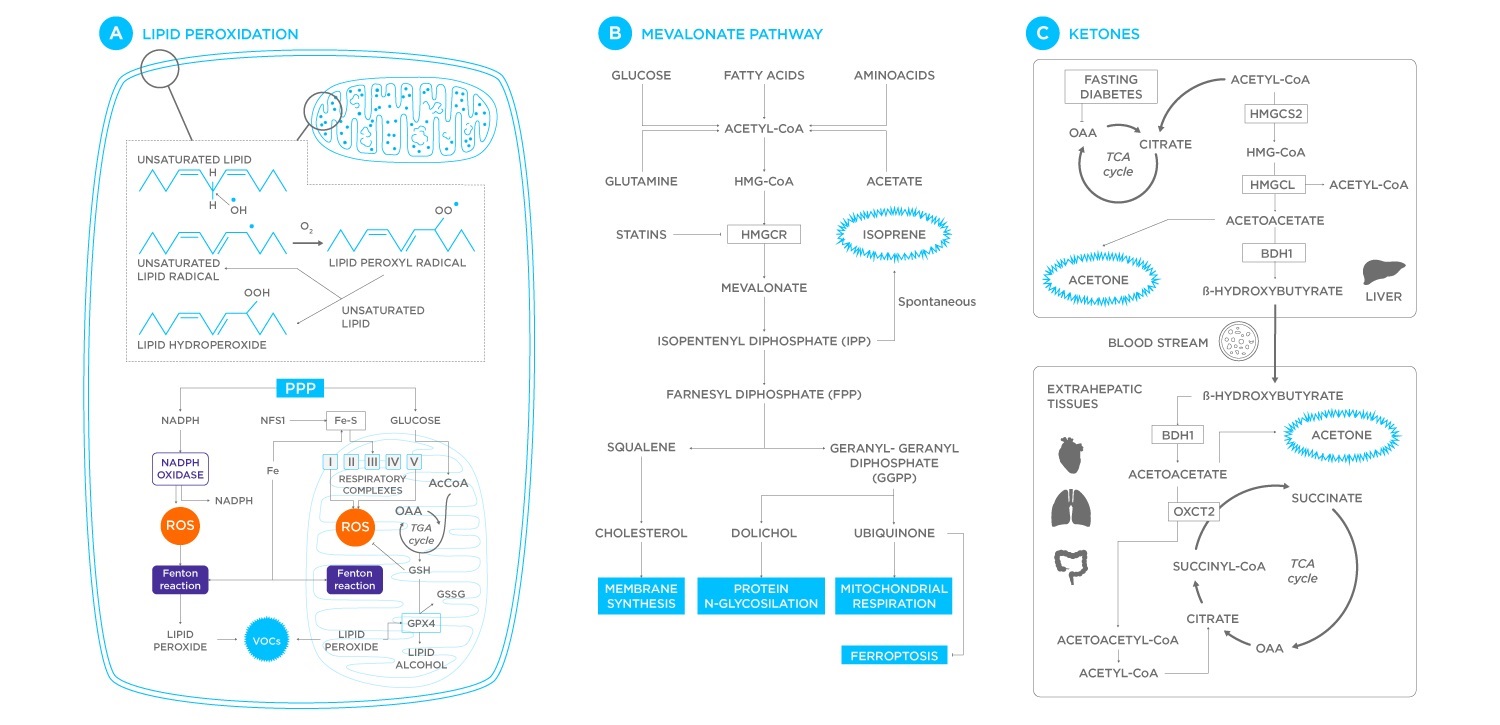
Figure 4. Metabolic pathways known to be relevant to the production of VOCs on breath. Lipid peroxidation related to oxidative stress produces various linear molecules, typically resulting in increases alkanes. The mevalonate pathway is involved in cholesterol synthesis and produces isoprene. While glucose insensitivity can lead to ketoacidosis, producing acetone.
While various VOCs have been reported in relation to cardiometabolic diseases, none have yet been fully characterized and validated for clinical use. Additionally, features of cardiometabolism, such as natriuretic peptide signaling, endoplasmic reticulum stress and changes in pro-inflammatory and pro-angiogenic activity are worthy of note and are yet to be associated with specific breath VOCs [19,20].
Breath Biopsy for Cardiometabolic Diseases
Non-invasive breath tests for cardiometabolic diseases would be easy to use for disease detection and monitoring with a wide range of patients including those who are morbidly obese. Breath sampling is also possible in a range of contexts and may even be suitable for at-home testing, making it ideal for ongoing health monitoring, which could be particularly useful where long-term lifestyle changes are needed (simple breath devices are currently used in this way to monitor gastrointestinal health). In the case of chronic heart failure, a breath test may also be relevant in predicting acute events and exacerbations.
We are the world-leader in Breath Biopsy® for early detection and precision medicine. Our Breath Biopsy products such as the ReCIVA® Breath Sampler are designed for reproducible and reliable collection of VOCs from human breath. Supported by expertise in study design, management, analysis and interpretation, our Breath Biopsy OMNI® service is the most advanced solution for global breath VOC analysis. Get in touch to discuss studying VOC biomarkers of cardiometabolic diseases using Breath Biopsy.
References
- WHO. The top 10 causes of death: World Health Organization; 2020 [updated 9th Dec 2020; cited 2021 13th Sept 2021]. Available from: https://www.who.int/news-room/fact-sheets/detail/the-top-10-causes-of-death
- National Academies of Sciences E, Medicine. High and Rising Mortality Rates Among Working-Age Adults. Washington, DC: The National Academies Press; 2021. English. (Harris KM, Majmundar MK, Becker T, editors.).
- WHO. Obesity and Overweight: World Health Organization; 2021. Available from: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight
- Malik VS, Willet WC, Hu FB. Nearly a decade on — trends, risk factors and policy implications in global obesity. Nature Reviews Endocrinology. 2020 2020/11/01;16(11):615-616. DOI: 10.1038/s41574-020-00411-y
- Coelho M, Oliveira T, Fernandes R. Biochemistry of adipose tissue: an endocrine organ. Arch Med Sci. 2013;9(2):191-200. DOI: 10.5114/aoms.2013.33181
- Davis CD. The Gut Microbiome and Its Role in Obesity. Nutr Today. 2016 Jul-Aug;51(4):167-174. DOI: 10.1097/NT.0000000000000167
- Walker RL, Vlamakis H, Lee JWJ, et al. Population study of the gut microbiome: associations with diet, lifestyle, and cardiometabolic disease. Genome Medicine. 2021 2021/12/17;13(1):188. DOI: 10.1186/s13073-021-01007-5
- Pereira J, Porto-Figueira P, Cavaco C, et al. Breath Analysis as a Potential and Non-Invasive Frontier in Disease Diagnosis: An Overview. Metabolites. 2015;5(1). DOI: 10.3390/metabo5010003
- Cikach FS, Dweik RA. Cardiovascular Biomarkers in Exhaled Breath. Progress in Cardiovascular Diseases. 2012 2012/07/01/;55(1):34-43. DOI: 10.1016/j.pcad.2012.05.005
- Biagini D, Lomonaco T, Ghimenti S, et al. Determination of volatile organic compounds in exhaled breath of heart failure patients by needle trap micro-extraction coupled with gas chromatography-tandem mass spectrometry. J Breath Res. 2017 Nov 29;11(4):047110. DOI: 10.1088/1752-7163/aa94e7
- Marcondes-Braga FG, Batista GL, Bacal F, et al. Exhaled Breath Analysis in Heart Failure. Current Heart Failure Reports. 2016 2016/08/01;13(4):166-171. DOI: 10.1007/s11897-016-0294-8
- Pham YL, Beauchamp J. Breath Biomarkers in Diagnostic Applications. Molecules. 2021;26(18):5514 DOI: 10.3390%2Fmolecules26185514
- Ferrandino G, Orf I, Smith R, et al. Breath Biopsy Assessment of Liver Disease Using an Exogenous Volatile Organic Compound—Toward Improved Detection of Liver Impairment. Clinical and Translational Gastroenterology. 2020;11(9):e00239. DOI: 10.14309/ctg.0000000000000239
- Murgia A, Ahmed Y, Sweeney K, et al. Breath-Taking Perspectives and Preliminary Data toward Early Detection of Chronic Liver Diseases. Biomedicines. 2021;9(11):1563. DOI: 10.3390/biomedicines9111563
- Sinha R, Lockman KA, Homer NZM, et al. Volatomic analysis identifies compounds that can stratify non-alcoholic fatty liver disease. JHEP Rep. 2020;2(5):100137-100137. DOI: 10.1016/j.jhepr.2020.100137
- Fernandez Del Rio R, O’Hara ME, Holt A, et al. Volatile Biomarkers in Breath Associated With Liver Cirrhosis – Comparisons of Pre- and Post-liver Transplant Breath Samples. EBioMedicine. 2015 Sep;2(9):1243-50. DOI: 10.1016/j.ebiom.2015.07.027
- O’Hara ME, Fernández Del Río R, Holt A, et al. Limonene in exhaled breath is elevated in hepatic encephalopathy. J Breath Res. 2016 Nov 21;10(4):046010. DOI: 10.1088/1752-7155/10/4/046010
- Khan MS, Cuda S, Karere GM, et al. Breath biomarkers of insulin resistance in pre-diabetic Hispanic adolescents with obesity. Sci Rep. 2022 Jan 10;12(1):339. DOI: 10.1038/s41598-021-04072-3
- Choi MR. Inside the pathophysiological mechanisms of cardiometabolic diseases: the other pandemic to fight. Pflügers Archiv – European Journal of Physiology. 2022 2022/01/01;474(1):1-4. DOI: 10.1007/s00424-021-02658-4
- Hess DA, Verma S, Bhatt D, et al. Vascular repair and regeneration in cardiometabolic diseases. Eur Heart J. 2022 Feb 10;43(6):450-459. DOI: 10.1093/eurheartj/ehab758
Catch up on the presentations from the Breath Biopsy Conference 2024
